How to Build a Patient Portal: The Complete Cost, Compliance, and Timeline Breakdown
Key Takeaways
- A patient portal built for compliance rather than usability will stall at 30–40% adoption, designed for the patient trying to message their doctor at 11 pm, not for the audit.
- Information blocking enforcement is now active in 2026, with ONC penalties reaching $1 million per violation annually; providers without adequate patient data access tools are already non-compliant.
- EHR integration will take longer and cost more than budgeted, every single time; each system (Epic, Oracle Health, Meditech) has its own implementation quirks on top of already complex data standards like FHIR R4 and HL7v2.
- Portals that get the core features right: secure messaging, lab results, and self-scheduling, see measurable returns: 21 million fewer no-shows and 30%+ faster bill collections.
Millions of Americans now have access to a patient portal. Only a third log in regularly. That’s not a technology problem; it’s a development problem.
Here’s a pattern we see constantly. A health system or startup builds a patient portal because the 21st Century Cures Act effectively mandates it. They check the compliance box. They launch. And then they watch adoption stall at 30-40% because the portal was designed for an audit, not for a patient trying to message their physician at 11 pm after a concerning lab result.
The global patient portal market was valued at USD 3.92 billion in 2024 and is projected to reach USD 8.38 billion by 2030, growing at a CAGR of 13.46%. That growth isn’t driven by curiosity; it’s happening because regulations are tightening and patient expectations are changing. More importantly, organizations that are getting patient portal development right are seeing measurable returns in engagement, retention, and operational efficiency.
This guide is not going to give you a list of items to tick and be done with. We will walk you through the compliance architecture required before you write a single line of code, what EHR integration actually costs, and why it consistently misses timelines. It will also detail the technology decisions that quietly determine whether your portal survives a security audit, and the mistakes that kill patient portal projects even after everything else goes right.
If you are planning to build a patient portal in 2026, this is what you really need to know before you even begin.
These guidelines apply across the board, from health systems launching their first digital patient experience to startups navigating the portal space, and from healthcare providers upgrading from underutilized legacy EHR platforms.
At Tech Exactly, we have been building healthcare applications — telemedicine platforms, EHR/EMR systems, remote patient monitoring apps, and, yes, patient portals — for more than a decade. This guide will cover everything you need to know before beginning patient portal development: the features that drive adoption, the compliance architecture that helps you avoid regulatory issues, what it realistically costs, and the timeline your stakeholders should expect.
Why Patient Portals Are Non-Negotiable in 2026
Three years ago, patient portal development was a nice-to-have. Today, it’s a regulatory requirement with real penalties for non-compliance.
The 21st Century Cures Act Changed Everything
The Cures Act Final Rule, enforced by the ONC, established information blocking provisions that prohibit healthcare providers from restricting patient access to their electronic health information (EHI).
As of February 2026, the HHS has begun active enforcement, meaning providers without adequate patient-facing data access tools are now subject to penalties and potential loss of certification.
In layman’s language, if your patients do not have access to their records, lab results, and clinical notes electronically, then you are already in violation
Putting this in perspective, the ONC can have health IT developers fined up to $1 million per violation annually for engaging in information blocking. This is no longer an empty threat. Enforcement is already active, and early penalty decisions are already establishing precedents.
CMS Interoperability Rules
The finalized CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F) mandates that payers implement patient access APIs and also utilize FHIR-based data exchange. This means patient portals can no longer just display information; they need to facilitate active, standardized data exchange across disparate healthcare systems.
The ROI Is Now Measurable
Research shows that patients with active portal accounts were 21.5% less likely to no-show, resulting in 21 million fewer missed appointments that year alone. That’s not a soft engagement metric. That’s revenue, care continuity, and operational capacity you can measure.
Patient Expectations Have Caught Up
According to ONC’s 2024 HINTS survey, 77% of individuals nationwide were offered online access to their health information in 2024 — up from 73% in 2022 — and 65% accessed their records at least once in the past year. Patient portal usage has more than doubled since the pre-pandemic rate of 15% in 2019.
Patients nowadays expect the same digital experiences from their healthcare provider as they get from their bank. A portal that requires multiple clicks to even see a single lab result is not going to survive.
It is one thing to be aware of the fact that you need a portal, but figuring out what to really build is where the budget becomes an issue. The data below highlights real patient utilization, and it also outlines the core functionalities that are needed for your minimum viable product (MVP) prior to further feature prioritization.
Let's Start Your Project Today
Ready to build your Patient Portal with us? Reach out now – our experts are just one click away.
Patient Portal Development: Must-Have Features for 2026
The key differentiating factor between a patient portal hitting 70%+ utilization and the one that gets abandoned is not the volume of integrated capabilities. It comes down to how well the right core functionalities are executed.
Must-Have Features (MVP)
Feature | What It Does | Why It Matters |
Secure Messaging | HIPAA-compliant communication between patients and care teams | Reduces phone call volume by 25-40%. Patients prefer async communication |
Lab Results & Clinical Notes | View test results, imaging reports, visit summaries, and physician notes | Required under the Cures Act. The #1 reason patients log into portals |
Appointment Scheduling | Self-service booking, rescheduling, and cancellation with automated reminders | Portal users had 21 million fewer no-shows in 2024 (Epic Research). This frees front-desk staff from phone scheduling |
Prescription Management | View active medications, request refills, track prescription history | Direct patient safety impact. Reduces medication errors |
Bill Pay & Insurance | View statements, make payments, check insurance coverage, download EOBs | Revenue cycle impact — online bill pay accelerates collections by 30%+ |
Patient Intake Forms | Digital pre-visit questionnaires, consent forms, demographic updates | Eliminates paper workflows. Saves 10-15 minutes per patient visit |
Accessibility is something every patient portal MVP needs, but it’s often pushed to the sidelines. WCAG 2.1 AA compliance is mandatory for healthcare apps meant for the general public. It’s not just about avoiding legal issues under ADA; it also directly impacts adoption, especially among older patients and people with disabilities, who tend to rely more on healthcare services.
Advanced Features (Phase 2+)
Feature | What It Does | Why It Matters |
Telehealth Integration | Launch video visits directly from the portal | Keeps patients in your ecosystem instead of losing them to third-party platforms |
Care Plan Access | View treatment plans, track goals, and log symptoms | Drives engagement for chronic disease management |
Proxy Access | Parents, caregivers, or legal guardians can manage another patient’s portal | Essential for pediatric and elderly care populations |
AI-Powered Symptom Triage | Pre-visit symptom assessment with routing recommendations | Reduces unnecessary ER visits. Improves clinical workflow efficiency |
Push Notifications | Alerts for new results, upcoming appointments, and ++++medication reminders | Drives repeat engagement. Mobile-first patients expect this |
Patient Education | Contextual health content linked to diagnoses and medications |
💡 Expert Tip:
Launching telehealth as a distinct product with an independent login significantly reduces patient engagement — the same friction that drives the telemedicine versus in-person care gap at the clinical level. The data indicates that patients are more likely to schedule follow-up video visits when a one-tap booking option is seamlessly integrated with their test results.
Because every additional step creates a barrier and decreases appointment conversion, telehealth needs to be integrated into the initial portal launch, rather than being deferred to subsequent phases.
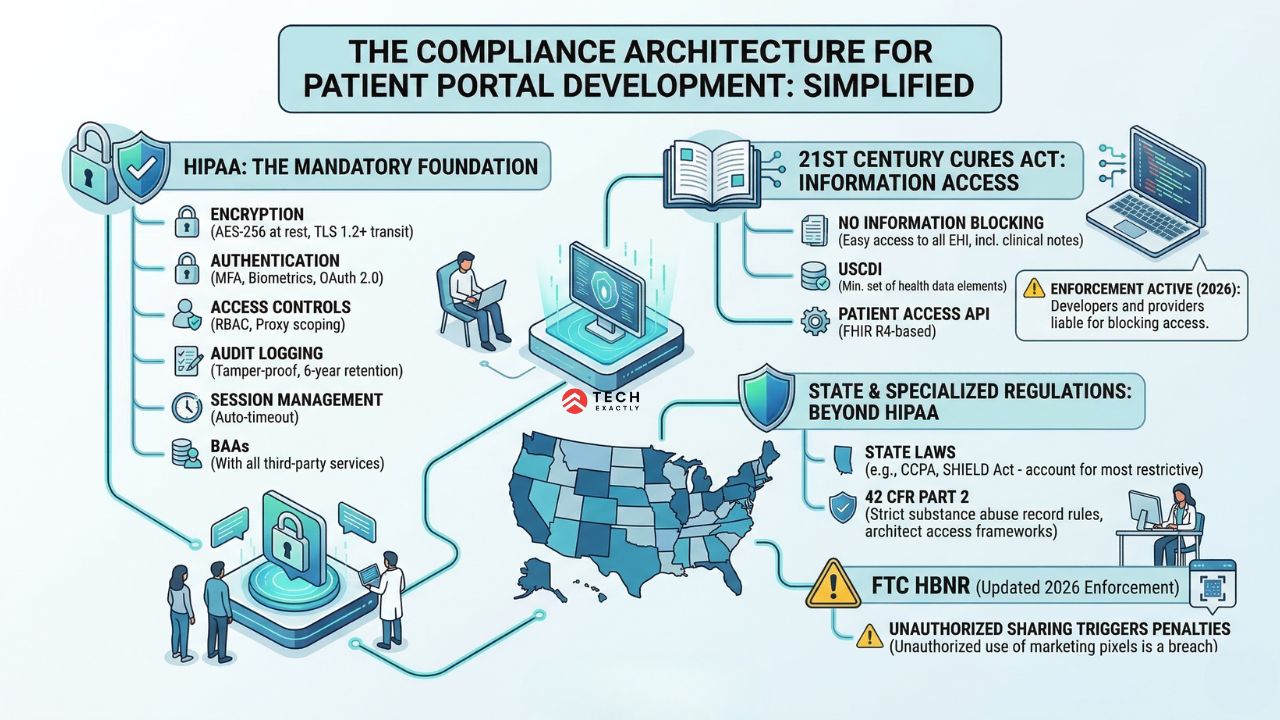
The Compliance Architecture for Patient Portal Development
The development of patient portal software faces a lot of strict regulatory needs in healthcare IT. If you fail to comply with these requirements, then it will result in heavy fines, lawsuits, and failed security audits.
HIPAA: The Foundation
Every patient portal handles Protected Health Information (PHI), which means HIPAA compliance isn’t optional and it is strictly mandatory. Here’s what that translates to architecturally:
Encryption: AES-256 for data at rest. TLS 1.2+ for data in transit. No exceptions — including database backups and log files.
Authentication: Multi-factor authentication (MFA) for all users. Biometric login (Face ID/fingerprint) for mobile. OAuth 2.0 or SAML for SSO with hospital identity providers.
Access Controls: Role-Based Access Control (RBAC) at minimum. Proxy access for caregivers needs separate permission scoping — a parent shouldn’t see their 18-year-old’s behavioral health notes.
Audit Logging: Every access to PHI must be logged with who, what, when, and from where. Logs must be tamper-proof and retained for a minimum of 6 years.
Session Management: Automatic timeout after inactivity (typically 15 minutes for clinical environments). Session tokens that can’t be reused across devices.
Business Associate Agreements: Every third-party service touching PHI — cloud hosting, push notification providers, analytics tools, employee management systems — needs a signed BAA.
▶️ See how we built a HIPAA-compliant web platform for an NYC therapy provider
21st Century Cures Act Compliance
Beyond HIPAA, your patient portal needs to comply with the information blocking provisions of the Cures Act:
No information blocking: It needs to be easy for the patients to be able to access all electronic health information (EHI) without there being unreasonable barriers. This will include clinical notes, the ones physicians used to keep internal
USCDI (United States Core Data for Interoperability): Your portal must support the USCDI v3 data standard, which defines the minimum set of health data classes and elements that must be available for patient access and exchange.
Patient Access AP: Organizations serving payers or CMS regulated entities must implement a FHIR R4-based Patient Access API. This will allow the patients and their authorized apps to securely retrieve claims, clinical records and formulary data.
💡 Expert Tip: Information blocking enforcement is now active as of 2026. The penalties hit health IT developers too, not just providers. If your portal software restricts patient access to EHI in a way that doesn’t fall under one of the eight recognized exceptions, you’re liable. Build for transparency from day one.
State-Level Regulations
Don’t forget that HIPAA is the floor, not the ceiling. For a wider view of healthcare app compliance across USA and UK, states like California (CCPA/CMIA), New York (SHIELD Act), and Texas (THIPA) have additional patient data protections that affect how your portal handles consent, breach notification, and data retention. If your patient portal serves patients in multiple states — and most do — your compliance architecture needs to account for the most restrictive state’s requirements.
A regulation that often blindsides portal teams is 42 CFR Part 2, which covers substance abuse records. If your portal handles behavioral health or substance use data, then the rules for sharing those records, especially around re-disclosure to other providers, are way stricter than HIPAA. It is imperative to architect your data access frameworks so that it accommodates these compliance standards before development rather than retroactively.
The FTC Health Breach Notification Rule (HBNR)
If your portal handles wellness data and it connects to wearable devices, or even if it operates outside traditional HIPAA rules, then you are an FTC target now. In 2026, the FTC is strictly enforcing its updated Health Breach Notification Rule (HBNR).
If you do unauthorized sharing of unidentified health information, including the use of marketing pixels, be it from Meta or Google, it automatically triggers federal penalties and also mandatory public disclosures.
Organizations can no longer rely on their non-covered entity status; if you handle the metrics, then your data must be completely locked down.
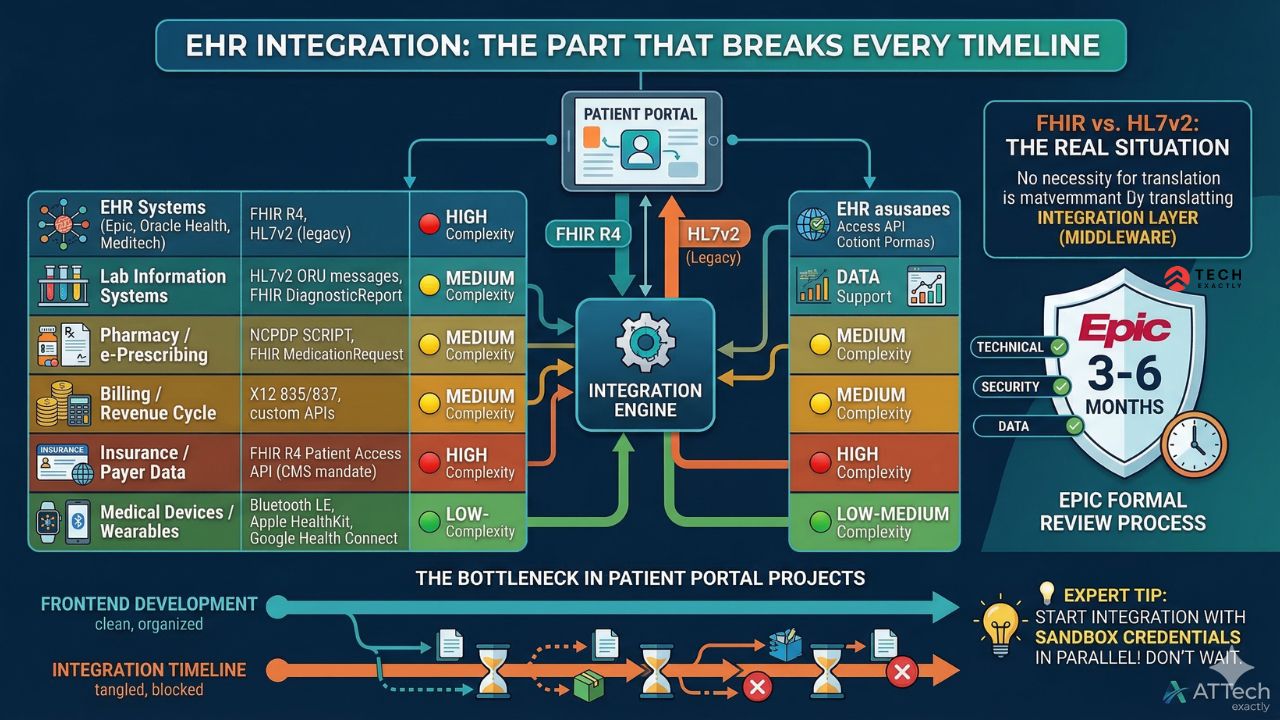
EHR Integration in Patient Portal Development
There is a universal truth in patient portal development: EHR integration is always going to take longer and be costlier than what you imagined or expected from day one.
The Integration Landscape
Your patient portal is not going to create clinical data randomly out of thin air by itself, it will pull from various sources like EHRs, lab systems, pharmacies, and billing platforms. The real struggle is that all of these systems speak a whole different language.
Integration Point | Data Standard | Complexity Level |
EHR Systems (Epic, Oracle Health, Meditech) | FHIR R4, HL7v2 (legacy) | 🔴 High — each EHR has implementation quirks |
Lab Information Systems | HL7v2 ORU messages, FHIR DiagnosticReport | 🟡 Medium — standardized but high data volume |
Pharmacy / e-Prescribing | NCPDP SCRIPT, FHIR MedicationRequest | 🟡 Medium — regulatory requirements for controlled substances |
Billing / Revenue Cycle | X12 835/837, custom APIs | 🟡 Medium — varies by clearinghouse and practice management system |
Insurance / Payer Data | FHIR R4 Patient Access API (CMS mandate) | 🔴 High — payer-specific FHIR implementations vary widely |
Medical Devices / Wearables | Bluetooth LE, Apple HealthKit, Google Health Connect | 🟢 Low-Medium — well-documented APIs, but data normalization is tricky |
FHIR vs. HL7v2: The Real Situation
While the Cures Act pushes FHIR R4 as the modern standard, the reality is that in 2026, most of the health systems still rely on HL7v2 for core transactions like ADT messages, labs, and pharmacy orders. The portal’s integration layer needs to handle both seamlessly.
This means building a middleware layer — an integration engine — that translates between HL7v2 and FHIR, normalizes data formats, and handles the edge cases that inevitably surface when you go from sandbox testing to production data. Budget 4-8 weeks for EHR integration alone.
Integrating your portal seems like a necessity for many, as Epic’s approximate 35% market share in US hospitals. It extends beyond just being a technical hurdle. It also needs to navigate a formal review process, which includes strict technical, security, and data evaluations.
This comprehensive process takes three to six months and operates entirely on Epic’s schedule, and you must initiate it before the development even begins or else your launch date will inevitably be delayed.
💡 Expert Tip: Start integration work with sandbox credentials in parallel with frontend development. Don’t wait until the UI is done. The integration timeline is the bottleneck in every patient portal project we’ve worked on — and waiting for production credentials from Epic or Oracle Health adds another 2-4 weeks on top.
How Much Does It Cost to Develop a Patient Portal?
Every founder or CTO eventually asks the same question: What does it actually cost to build a custom patient portal development? For broader context across types of healthcare apps and their development challenges, cost depends heavily on the scope of compliance requirements and the complexity of the integration. Below is a breakdown of what you should expect
| Portal Complexity | What’s Included | Estimated Cost | Timeline |
| Basic Portal | Secure messaging, lab results, appointment scheduling, bill pay. Single EHR integration. HIPAA compliance. Responsive web. | $80,000 – $150,000 | 4-6 months |
| Mid-Range Portal | Everything above + telehealth integration, prescription management, care plan access, proxy access. Multiple EHR integrations. Mobile app (iOS + Android). | $150,000 – $250,000 | 6-9 months |
| Enterprise Portal | Full feature set + AI-powered triage, wearable device integration, multi-language support, white-label customization, advanced analytics dashboard for providers. | $250,000 – $400,000+ | 9-14 months |
Where the Money Actually Goes
| Cost Component | % of Total Budget | Why |
| EHR Integration | 25-35% | The most complex and unpredictable line item. Multiple EHR systems multiply this cost. |
| Compliance & Security | 15-25% | HIPAA architecture, penetration testing, audit logging, encryption infrastructure, and compliance documentation. |
| Frontend Development | 15-20% | Patient-facing UI (web + mobile), provider-facing dashboards, responsive design. |
| Backend / API Layer | 15-20% | Core business logic, data processing, FHIR/HL7 middleware, notification services. |
| UX/UI Design | 5-10% | Workflow mapping, clinical user research, accessibility (WCAG 2.1 AA), and prototype iteration. |
| QA & Testing | 5-10% | Functional, security, compliance, interoperability, and clinical workflow testing. |
| Project Management | 5-8% | Coordination across compliance, development, and integration teams. |
Cost Variables That Shift the Number
Before you start evaluating for custom development, you need to ensure it is actually the right choice. If you are a single specialty practice on Epic without multi-EHR needs or proprietary feature plans, MyChart seems to be sufficient.
Custom portals make financial sense only when you need multi-EHR integration, specialized branding, advanced functionalities like AI triage, or when developing a multi-provider SaaS platform. Otherwise, a custom build solves a problem that you never really had.
- Number of EHR integrations: Every single additional EHR system adds $20,000-$50,000 in integration work.
- Mobile app development: A native iOS + Android app adds $40,000-$80,000 over a responsive web-only portal. Cross-platform frameworks like React Native or Flutter can reduce this by 30-35%.
- AI features: Adding AI-powered functionality like symptom triage, intelligent appointment routing, or clinical documentation summarization adds $30,000-$60,000, depending on complexity.
- Multi-tenant architecture: Building for multiple provider organizations (SaaS model) adds architectural complexity and 15-20% to total cost.
For a detailed and thorough breakdown across all app types, you should definitely see our healthcare app development cost guide.
Let's Start Your Project Today
Ready to build your Patient Portal with us? Reach out now – our experts are just one click away.
Patient Portal Development Timeline: Phase by Phase
Here’s what a realistic timeline looks like for a mid-range patient portal with EHR integration and mobile app support:
Phase | Duration | Key Activities |
Phase 1: Discovery & Compliance Scoping | 3-5 weeks | Requirements gathering, compliance assessment, EHR integration scoping, data flow mapping, security architecture planning |
Phase 2: UX Design & Clinical Workflow Mapping | 4-6 weeks | User research with patients AND providers, wireframing, prototype testing, WCAG accessibility audit, design system creation |
Phase 3: Backend & Integration Development | 8-12 weeks | Core API development, FHIR/HL7 integration engine, database architecture, authentication/authorization, encryption infrastructure |
Phase 4: Frontend Development | 6-10 weeks | Patient-facing web portal, mobile app (iOS + Android), provider dashboard, responsive design implementation |
Phase 5: EHR Integration & Testing | 4-8 weeks | Sandbox testing, production credential acquisition, data validation, edge case handling, performance testing |
Phase 6: Security & Compliance Testing | 3-5 weeks | Penetration testing, HIPAA compliance validation, vulnerability scanning, interoperability testing, clinical workflow validation |
Phase 7: Launch & Post-Launch | 2-3 weeks | Staged rollout, monitoring setup, incident response plan activation, user onboarding, feedback collection |
Total: 6-9 months for a fully integrated patient portal with mobile apps.
⚠️ Reality Check: While it is true that timelines often assume that EHR vendors are going to provide sandbox and production credentials within 2-4 weeks, and on the other hand, Epic and Oracle Health usually take around 4-8 weeks. You need to account for this extended duration during project planning, as it represents the primary catalyst for schedule delays in patient portal deployments.
Technology Decisions That Shape Your Patient Portal
Web vs. Mobile vs. Both
Most patient portal interactions happen on mobile — the Pew Research Center reports that 97% of Americans own a cellphone, with 90% owning a smartphone. But providers and administrative staff interact with portal dashboards on the desktop. The answer is almost always both: a responsive web application plus native or cross-platform mobile apps.
We typically recommend React Native for patient portal mobile development — the shared codebase between iOS and Android reduces development time by roughly 35%, and the performance is more than adequate for the data-display and communication features that dominate portal usage. For a deeper comparison, see our tech stack guide for healthcare apps.
Cloud Infrastructure
Patient portal hosting must be HIPAA-eligible with a signed BAA. The three realistic options:
AWS (most common in healthcare IT — broadest BAA coverage, mature FHIR tooling via HealthLake)
Azure (strong Azure Health Data Services with native FHIR Server, good fit for Microsoft-heavy organizations)
Google Cloud (Healthcare API with FHIR store, strong ML capabilities for AI-enhanced portals)
AI Integration Opportunities
Generative AI is transforming healthcare applications, and patient portals are a prime deployment target. Practical AI features for portals include:
Intelligent symptom triage: Pre-visit assessment that routes patients to the right care level (ER vs. urgent care vs. telehealth vs. self-care)
Lab result explanations: Plain-language summaries of clinical data using LLMs, with appropriate disclaimers
Smart scheduling: Matching appointment duration and provider specialty to patient-reported symptoms
Agentic AI workflows: Automated follow-up reminders, care gap identification, and proactive outreach based on patient data patterns
💡 Expert Tip #1: If you’re adding AI features that interpret clinical data or make care recommendations, review the FDA’s guidance on Clinical Decision Support software carefully. Some AI features may trigger SaMD classification and require regulatory clearance.
💡 Expert Tip #2: Under the ONC HTI-1 Transparency Mandate, the portals are being used for predictive AI or Decision Support Interventions (DSI) like symptom triage or risk scoring, which is in conjunction with certified EHRs. This regulation makes it mandatory to add an “AI nutrition label” right there within the user interface, explicitly detailing your training data, known biases, and validation metrics. In 2026, Blackbox AI is now dead when it comes to clinical settings, and transparency is legally required.
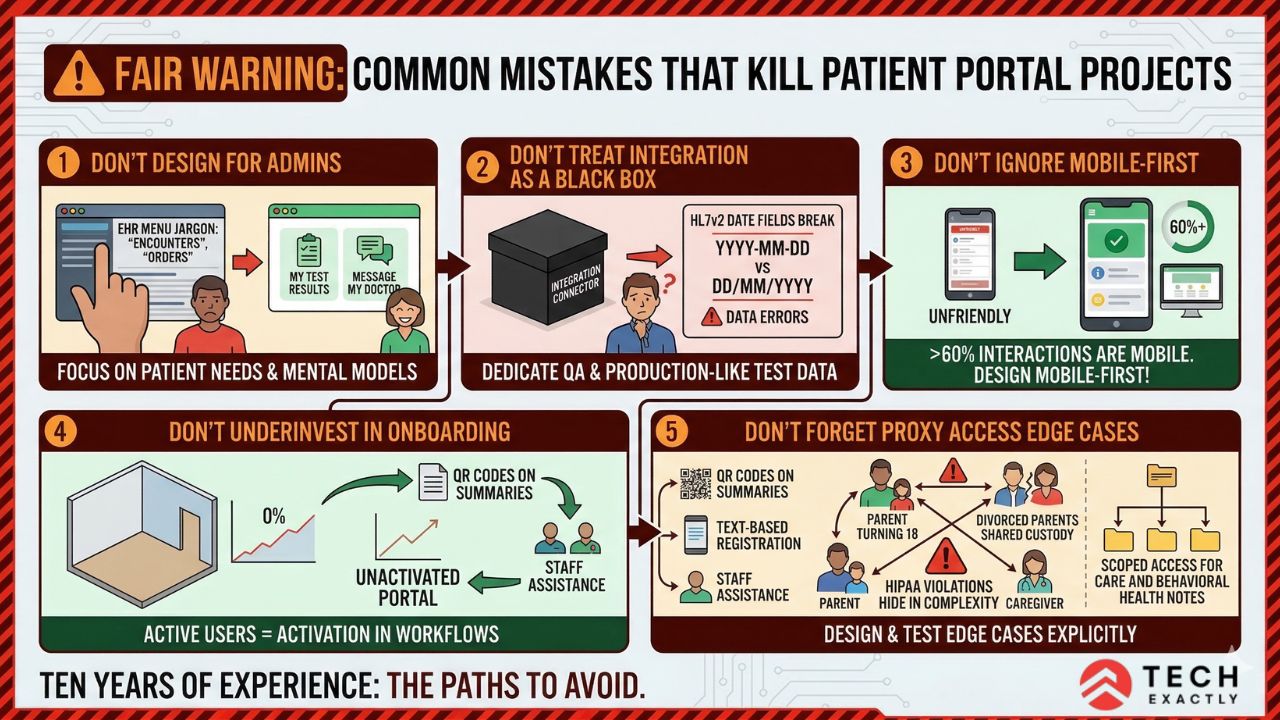
Mistakes to Avoid While Building Patient Portals
After building healthcare applications for over a decade, these are the patterns that doom patient portal development:
Designing for the admin, not the patient. If you replicate an EHR’s menu structure for your portals’ navigation is a guaranteed way for you to end up losing users. Patients do not care about clinical jargon like ‘encounters’ or ‘orders’ all they want is to find “my test results” and “message my doctor”. You need to stop forcing clinical mental models onto regular, everyday patients.
Treating EHR integration as a black box. Teams that hand off integration to a “connector” and assume it works are the teams that discover — three months into production — that HL7v2 lab messages from one hospital format date fields differently than another. Integration needs dedicated QA resources and production-like test data.
Ignoring mobile from the start. Building a desktop-first portal and then trying to make it responsive is expensive rework. The majority of patient portal interactions happen on mobiles. So, design mobile-first.
Underinvesting in onboarding. You can build the greatest patient portal on Earth, but it is still going to be completely worthless if users fail to even activate their accounts. You need to stop waiting for patients to find it. You need to integrate activation right there into clinical workflows using QR codes on after-visit summaries, text-based registration at intake, and staff-assisted setup for those who are going to need technical help.
Forgetting about proxy access edge cases. A parent managing a child’s portal account sounds simple until that child turns 18, or divorced parents have shared custody, or a caregiver needs access to an elderly parent’s records but not their behavioral health notes. These edge cases need to be designed and tested explicitly — they’re where HIPAA violations hide.
What Comes Next
Patient portal development is at a critical turning point. The current regulatory landscape that is driven by Cures Act enforcement, CMS interoperability mandates, and TEFCA is driving the industry toward open, patient-first data access. Organizations that build a portal’s architecture to accommodate this shift right now will be securing a substantial competitive advantage.
The portals that win adoption won’t be the ones with the longest feature list. They’ll be the ones that make it genuinely easier for a patient to manage their health digitally than to pick up a phone. That requires understanding clinical workflows, not just writing code. More importantly, it requires a development partner that has built healthcare software before.
If you’re planning a patient portal and want to understand what the compliance architecture, integration scope, and realistic timeline look like for your specific use case, we offer a free consultation to map it out.
Let's Start Your Project Today
Ready to build your Patient Portal with us? Reach out now – our experts are just one click away.
FAQs About Patient Portal Development
A basic patient portal with single EHR integration and HIPAA compliance starts at $80,000-$150,000. A mid-range portal with telehealth, mobile apps, and multiple EHR integrations runs $150,000-$250,000. Enterprise portals with AI features, wearable integration, and multi-tenant architecture can exceed $400,000. For context across all healthcare app types, see our healthcare app development cost guide.
A basic development timeline usually ranges from four to six months for a foundational web portal featuring just a single EHR integration. And if you add mobile apps and multiple integrations, then it extends to 6-9 months, while massive enterprise builds can also take around 9-14 months. The biggest delay is EHR vendor credentialing: simply getting production API access from Epic or Oracle Health can also take up to 4-8 weeks.
At minimum: HIPAA (Privacy Rule, Security Rule, Breach Notification Rule) for any portal handling Protected Health Information. The 21st Century Cures Act requires patient access to all electronic health information without information blocking. State-level regulations (CCPA, SHIELD Act, etc.) may add additional requirements. If your portal serves CMS-regulated payers, the CMS Interoperability Final Rule requires FHIR-based Patient Access APIs.
EHR vendor portals (MyChart by Epic, Oracle Health Patient Portal) offer really quick deployment but also have limited customization. Custom patient portal development makes much more sense when you need: a branded experience, integration across multiple EHR systems, advanced features like AI triage or telehealth, support for specific patient populations, or a SaaS product serving multiple provider organizations. Many health systems run a custom portal alongside their EHR's native portal for different use cases.
Yes, if you’re working with any entity under the Cures Act or CMS rules which is usually every US provider and payer, FHIR R4 is the mandatory standard law for patient data APIs. Even if you begin with HL7v2, building a FHIR-native architecture from the very first day prevents expensive redesigns later.
The data is hard to argue with. Epic Research found that patients with active portals had a no-show rate of just 6.2% compared to 7.9% without one — translating to 21 million fewer missed appointments in 2024 alone. Beyond no-shows, organizations report reduced call center volume (secure messaging displaces 25-40% of phone calls), faster revenue collection (online bill pay accelerates payment by 30%+), and improved patient satisfaction scores. The health insurance app integration component alone can significantly impact revenue cycle efficiency.
Ready to Get Started?
Get a free quote and see what we can do for you.
Pallabi Mahanta, Senior Content Writer at Tech Exactly, has over 5 years of experience in crafting marketing content strategies across FinTech, MedTech, and emerging technologies. She bridges complex ideas with clear, impactful storytelling.
