EHR Integration: Why It Eats Half Your Budget and How to Fix That
Key Takeaways
- EHR integration eats 15–30% of your total healthcare app budget, and most teams don’t realize it until they’re already committed
- Epic certification alone takes 3–6 months and ~$10K per round. Factor that into your timeline before you promise a launch date
- Middleware platforms like Redox (~$45K/year for startups) can cut months off your integration timeline if you need multiple EHR vendors
- The architecture decisions you make in Week 1 determine 70% of total integration cost. Scope it early or pay for it later
You budgeted four weeks for EHR integration. You’re now in month three, and your team just found out the hospital’s lab system still runs HL7v2 messages from 2009.
If that sounds familiar, you’re in good company. EHR integration is the single most underestimated line item in healthcare app development. It regularly consumes 15-30% of your total project budget. About 40% of healthcare leaders say that their implementation efforts run into serious issues.
The issue isn’t that integration is hard. The problem is that most teams don’t realize how hard it is until they are already knee-deep in it. And by that point, the decisions that determine 70% of the total cost are already made.
Here’s where the money actually goes, why timelines blow up, and how to approach EHR integrations without draining your budget.
Why EHR Integration Costs So Much
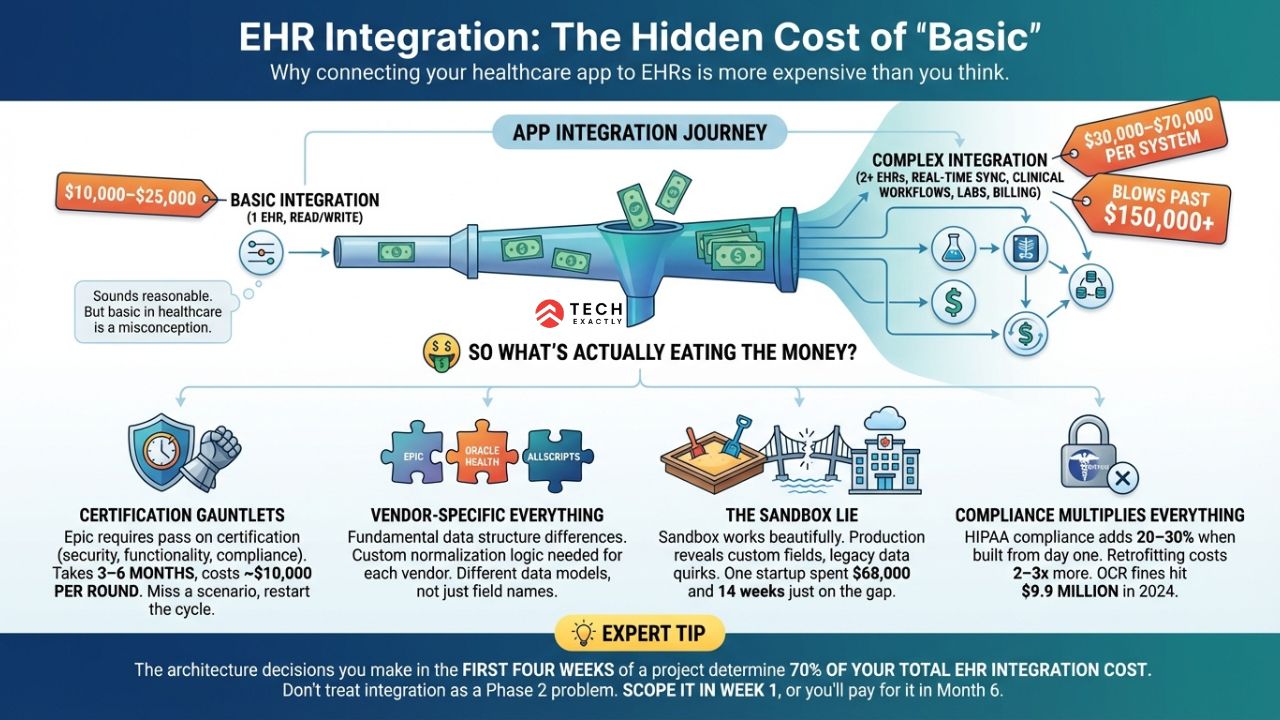
Connecting your app to a single EHR for read/write access costs $10,000–$25,000. Sounds reasonable. But basic in healthcare is a misconception.
The second you need two-way data flow, multiple EHR vendors, real-time sync, or anything touching clinical workflows, you’re looking at $30,000–$70,000 per system. Add in labs, imaging, billing, and third-party services, and it blows past $150,000.
So what’s actually eating the money?
Certification Gauntlets. You don’t just build an integration and launch it. Epic requires every app to pass its certification process, which includes security reviews, functionality testing, and compliance validation. That process takes 3–6 months and costs roughly $10,000 per certification round. Miss a scenario in testing, and you have to restart the cycle.
Vendor-specific Everything. Epic’s patient data structure is fundamentally different from Oracle Health’s, which differs from Allscripts’. These aren’t just minor field name variations. They are different data models that require custom normalization logic for each vendor. Your EHR integration API layer needs to handle all of them.
The Sandbox Lie. Every major EHR vendor offers a sandbox environment for developers. The sandbox works beautifully. Then you move to production and discover that the hospital’s instance has custom fields, legacy data formats, and configuration quirks that the sandbox never surfaced. One startup reported spending $68,000 and 14 weeks just to get two EHR integrations live. Surprisingly, most of that time was burned in the gap between sandbox and production.
Compliance multiplies everything. HIPAA compliance adds 20–30% to development costs when built from day one. Retrofitting it later costs 2–3x more. The stakes are high and real. OCR hit healthcare organizations with $9.9 million in HIPAA fines in 2024, more than double the previous year.
💡 Expert Tip: The architecture decisions you make in the first four weeks of a project determine 70% of your total EHR integration cost. Don’t treat integration as a Phase 2 problem. Scope it in Week 1, or you’ll pay for it in Month 6.
Let's Start Your Project Today
Ready to set up your EHR Integration with us? Reach out now – our experts are just one click away.
EHR Integration Standards: HL7v2 vs FHIR in 2026
Every founder we talk to asks the same thing: “Can’t we just use FHIR?”
Sure. But you’ll also need HL7v2. Here’s why.
HL7v2 is a messaging standard from the 1990s that still runs inside the majority of US healthcare organizations. In most hospitals, lab results, billing, and scheduling, which is the operational backbone, still run on HL7v2. It’s not elegant. It’s not modern. But it works, and hospitals aren’t replacing it anytime soon.
FHIR (Fast Healthcare Interoperability Resources) is the modern standard with RESTful APIs, JSON payloads, and clean resource models. More hospitals now support FHIR-enabled apps than ever before. The 21st Century Cures Act mandates FHIR support in certified EHRs. Adoption is accelerating globally. About 73% of countries with health data regulations now mandate or advise FHIR use.
Here’s the part nobody puts in the sales pitch: 84% of hospitals that technically support FHIR still struggle with seamless data exchange. “FHIR-compliant” on paper and “actually interoperable” in production are wildly different things. One vendor omits optional fields. Another uses a different code system for the same data. A third might reorder payloads just enough to break your parsing logic in the middle of the night.
What this means for your build: Your EHR data integration layer needs to speak both languages. FHIR for modern API access, HL7v2 for the legacy systems that aren’t going anywhere. Plan for both from the start.
Epic vs Oracle Health: What Each Integration Actually Looks Like
Between them, these two own 65% of the acute care EHR market. If you’re building a healthcare app, odds are you’ll deal with one or both.
Epic EHR Integration (42.3% Market Share)
Epic’s developer program starts at $100/year for sandbox access. But getting to production is where the cost and timeline live.
The certification process takes 3–6 months. Every app must pass security reviews and functionality testing. The initial interface setup runs $15,000–$20,000 before you start working on real patient data. Epic supports FHIR, SMART on FHIR, and CDS Hooks. However, their implementation has Epic-specific complexities that the documentation doesn’t always surface.
On the AI front, Epic is moving fast. 62.6% of Epic hospitals have adopted ambient AI documentation tools. At their 2025 user group meeting, Epic showed AI agents like “Art” for clinician visit prep and “Emmie” as a patient-facing MyChart chatbot.
Oracle Health / Cerner EHR Integration (22.9% Market Share)
Oracle Health is more accessible upfront. API docs and best practice guides are free. A one-time $10,000 fee gets you certified API access to one production and one non-production environment.
Compared to Epic builds, integrations are usually 15–20% less time-consuming, partly because Oracle’s hosting is more centralized. They support FHIR R4, HL7v2 via Cerner Open Interface, and their proprietary Millennium APIs.
The catch? Oracle Health is still in transition. After the $28.3 billion acquisition, 12 of Cerner’s biggest clients walked. The platform itself is stable, but the ecosystem around it is shifting. If you’re betting your product on Oracle Health long-term, be vigilant.
💡 Expert Tip: Don’t pick your first EHR integration based on which vendor is “easier.” Pick the one your target customers actually use. If you’re building for small practices, it might be Athenahealth or DrChrono. If you’re targeting hospitals, it’s Epic or Oracle Health. Your market determines your integration roadmap and not your engineering preference.
EHR Integration Solutions: The Middleware Shortcut
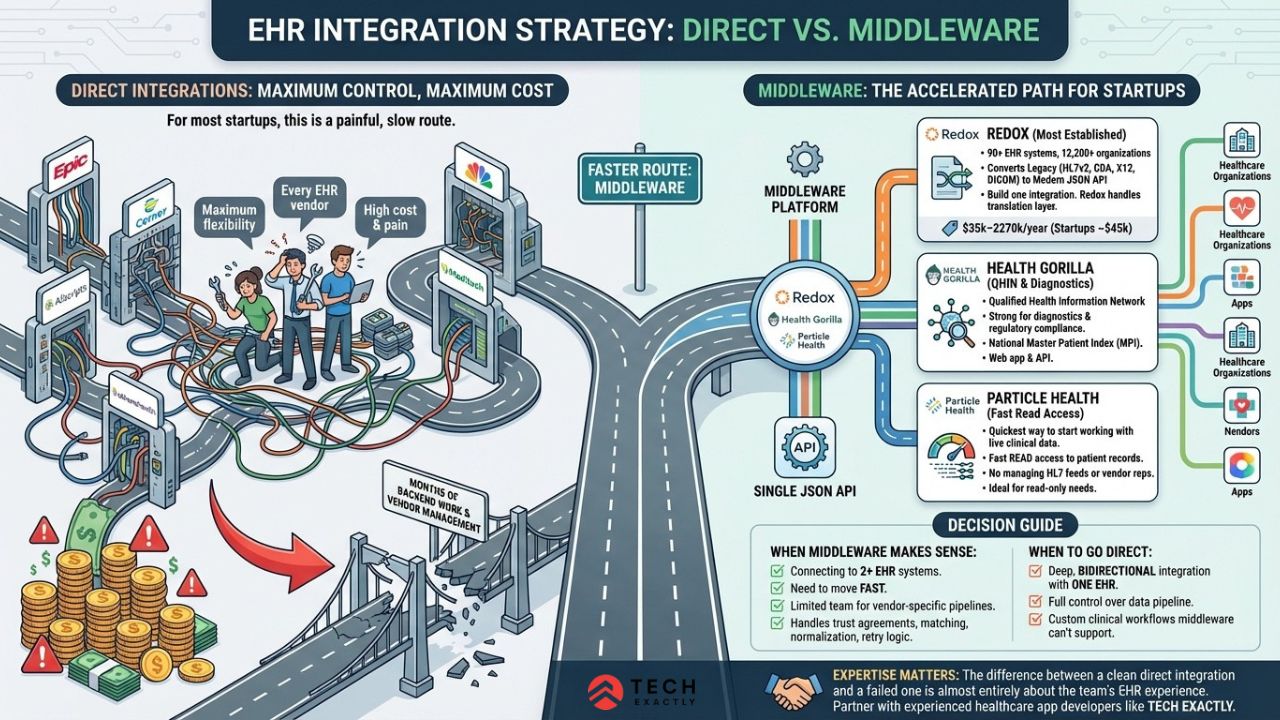
You could build direct integrations to every EHR vendor. Maximum flexibility. This also means maximum cost and pain. For most startups and smaller teams, middleware gets you there faster.
Redox is the most established player, connected to 90+ EHR systems across 12,200+ healthcare organizations. They convert legacy formats (HL7v2, CDA, X12, DICOM) into a modern JSON API. Thus, you build only one integration, and Redox handles the translation layer for each EHR. Pricing starts at $35,000–$270,000/year, depending on volume, with startups typically landing around $45,000/year.
Health Gorilla operates as a Qualified Health Information Network (QHIN) and is strong for diagnostics and regulatory compliance use cases. They facilitate data exchange via both a web app and API, with a national Master Patient Index for patient matching.
Particle Health is built for fast read access to patient records. It’s one of the quickest ways to start working with live clinical data without managing HL7 feeds or dealing with EHR vendor reps. It’s not as strong for bidirectional exchange, but if your app mainly needs to read patient data, it can be a very practical option.
When middleware makes sense: You’re a startup connecting to 2+ EHR systems, you need to move fast, and you don’t have the team to manage vendor-specific integration pipelines. Middleware platforms handle the trust agreements, patient matching, data normalization, and retry logic that would otherwise eat months of backend work.
When to go direct: Your product requires deep, bidirectional integration with a single EHR vendor, you need full control over the data pipeline, or your use case requires custom clinical workflows that middleware can’t accommodate. This is where working with an experienced [healthcare app development company like Tech Exactly matters. The difference between a clean direct integration and a failed one is almost entirely about the team’s EHR experience.
AI and EHR Integration: What's Working Right Now
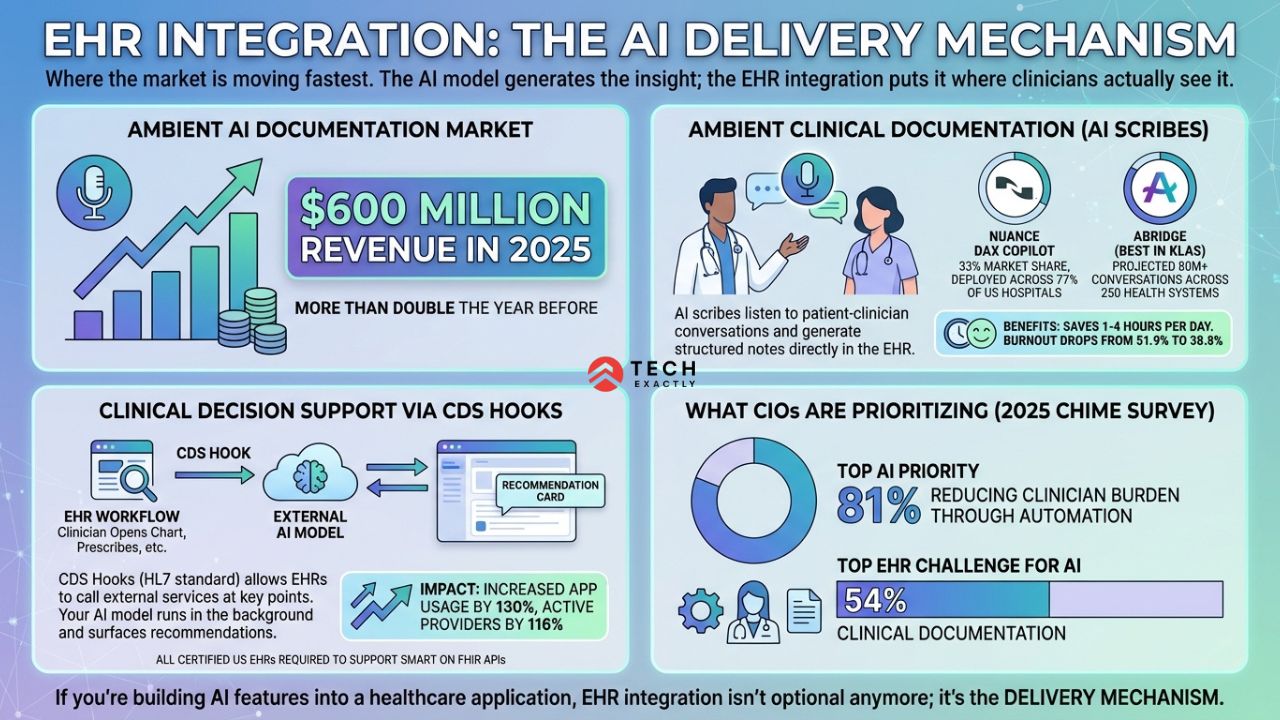
This is where the market is moving fastest. The ambient AI documentation market alone pulled in roughly $600 million in revenue in 2025, which is more than double the year before.
Here’s what’s actually running in production, not just in press releases:
Ambient clinical documentation. AI scribes that listen to patient-clinician conversations and generate structured notes directly in the EHR. Nuance DAX Copilot holds 33% market share, deployed across 77% of US hospitals. Abridge, which is named Best in KLAS for 2025 and 2026, is projected to support 80 million+ patient conversations across 250 health systems. Physicians who use these tools save 1-4 hours per day. According to a study of 263 physicians across six health systems, burnout rates dropped from 51.9% to 38.8%.
Clinical decision support via CDS Hooks. CDS Hooks is an HL7 standard that allows EHRs to call external services at key points in the workflow, like when a clinician opens a patient chart, prescribes medication, or places an order. Your AI model runs in the background and surfaces recommendations as cards within the EHR interface. In clinical trials, CDS Hooks interventions increased app usage by 130% and active providers by 116%. All certified US EHRs are required to support SMART on FHIR APIs, making this the most scalable path for AI-driven EHR integration.
What CIOs are prioritizing. Surveys indicate that 81% of healthcare CIOs say their top AI priority is reducing clinician burden through automation. 54% specifically name clinical documentation as the top EHR challenge AI could solve.
If you’re building AI features into a healthcare application, EHR integration isn’t optional anymore; it’s the delivery mechanism. The AI model generates the insight. The EHR integration puts it where clinicians actually see it.
Let's Start Your Project Today
Ready to set up your EHR Integration with us? Reach out now – our experts are just one click away.
How to Keep EHR Integration From Blowing Your Budget
Scope integration in Week 1, not Phase 2. Talk to the EHR vendors your customers use before you write a line of code. Understand their API capabilities, certification requirements, and timeline. Too many startups build the product first and only later discover that their target EHR can’t support the data access they need.
Start with one EHR, one direction. Don’t try to integrate with Epic, Oracle Health, and Athenahealth simultaneously. Pick the vendor your first three customers use. Build a clean, well-tested read integration first. Add write access after you’ve validated the data flow. Expand to additional vendors only when customer demand justifies it.
Evaluate middleware before going direct. If you need to support multiple EHRs and you’re pre-Series A, the $45,000/year for Redox is likely cheaper and faster than building direct integrations at $30,000–$70,000 per vendor. You can always replace middleware with direct integrations later as you scale and need more control.
Budget for the post-sandbox surprise. Whatever your integration estimate is, add 20–30% for the gap between sandbox and production. Every production EHR setup has custom fields, old data issues, and unexpected configuration problems that sandbox testing won’t catch.
Don’t build compliance later. HIPAA, HITECH, and the new 2025 Security Rule changes are non-negotiable. Retrofitting compliance costs 2–3x more than building it in from day one. Encrypt data at rest and in transit, implement audit logging, and ensure all Business Associate Agreements (BAAs) are signed before working with production data.
Ready to Integrate With EHR Systems Without the Budget Blowout?
EHR integration doesn’t have to be the thing that blows up your budget. What it needs is a solid team that can handle vendor certification calls, can debug HL7v2 messages at midnight, and knows where production issues can arise from.
We’ve done this at Tech Exactly for health tech startups shipping their first product and growing practices connecting to multiple EHR systems. We define integration requirements from the start, so you’re not forced into last-minute fixes later in the build.
Let's Start Your Project Today
Ready to set up your EHR Integration with us? Reach out now – our experts are just one click away.
FAQs About EHR Integration
A basic single-system integration costs $10,000–$25,000. Mid-complexity integrations (bidirectional data, clinical workflows) cost $30,000–$70,000 per system. Complex multi-system integrations with labs, imaging, and billing can exceed $150,000. Middleware platforms like Redox offer an alternative at $35,000–$80,000/year for access to 90+ EHR systems.
Epic integrations take 3-6 months, and Oracle Health integrations a little less. Middleware-based integrations take a few weeks and not months. The biggest variable is the gap between sandbox testing and production, which is where unexpected issues almost always show up.
HL7 v2 is an established but legacy standard from the 1990s, still used by about 95% of U.S. healthcare organizations for their workflows. On the other hand, FHIR is the latest standard, featuring RESTful APIs and JSON-based data formats, and is mandated by the 21st Century Cures Act. Most health tech applications need to support both, since hospitals typically use HL7 v2 internally while exposing FHIR APIs externally.
When you don't have a team for vendor-specific integration workflows, and still you need to support multiple EHR integrations, Middleware (Redox, Health Gorilla, Particle Health) is your best choice. Go direct when you need deep, bidirectional integration with a single vendor or when your use case requires custom clinical workflows.
Yes, you can. In fact, it is the fastest-growing segment in health tech. The most common use case today is ambient AI documentation with tools that listen during visits and automatically write notes into the EHR. For use cases like clinical decision support, CDS Hooks and SMART on FHIR make it possible to surface AI-generated recommendations directly within the EHR workflow. All certified U.S. EHRs are required to support these standards.
At Tech Exactly, we offer a full integration lifecycle, from scoping which EHR vendors your customers use to certification and production deployment. We work with FHIR, HL7v2, and vendor-specific APIs (Epic, Oracle Health, Athenahealth, and others), and we build HIPAA-compliant data pipelines that pass vendor certification on the first round whenever possible.
Manas Das, Mobile App Architect at Tech Exactly, has over 9 years of experience leading teams in iOS, Android, and cross-platform development. He specialises in scalable app architecture and GenAI-driven mobile innovation.
