Custom Healthcare Software: Build vs Buy for Startups

Key Takeaways
- Compliance isn’t a layer you add later; your entire architecture must be HIPAA-compliant from day one, since a single overlooked provision can result in fines up to $2.1 million per violation category annually.
- Regulatory missteps go beyond HIPAA, a missed IEC 62304 classification can stall an FDA submission for months, and EHR integrations involving legacy HL7v2 systems can consume half your budget if not planned for upfront.
- There’s no such thing as “HIPAA certification”; what exists is HIPAA compliance, validated through third-party audits like HITRUST or SOC 2 Type II. Anyone selling you a certification badge is not delivering an actual standard.
- Understanding the clinical environment is just as critical as writing good code; teams that ignore how healthcare workflows actually function will see that gap reflected directly in the final build.
Within the first six months, every healthcare startup faces the question of whether to invest in custom healthcare software development or just buy something off the shelf and further customise it. The answer sounds simple. But never is.
If you buy too early, you will end up fighting a platform for the next two years that wasn’t built for your workflow. If you build too early, you will end up burning your runway solving problems that Athenahealth already solved years ago. A wrong decision doesn’t just cost money; it also costs time, which you can’t get back in this fast-changing market. The money flowing into digital health is real, about $14.2 billion in 2025 alone. But so is the pressure to deliver. And that pressure is where the build-vs-buy decision gets made badly.
Here’s how to think about it clearly.
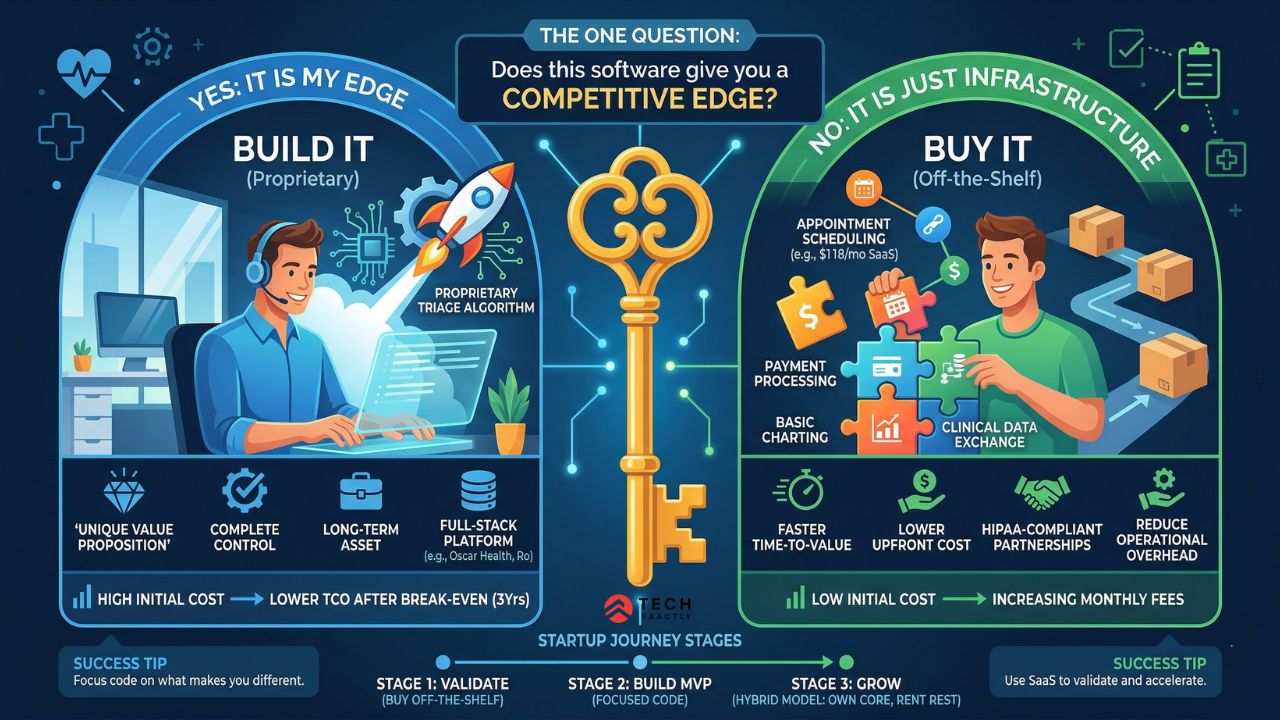
Custom Healthcare Software Development: Build or Buy Comes Down to One Question
If software is something that gives you a competitive edge over every other player in this space, you build it. If software is just infrastructure that supports your actual product (which might be a care model, a clinical protocol, a network), you buy it.
Think about it this way: if you’re a founder building a telemedicine platform with a proprietary triage algorithm, that algorithm is your edge, and hence, you build it. But the appointment scheduling, payment processing, and basic charting underneath it? That’s just integration. So, you buy it.
Companies like Oscar Health and Ro built full-stack platforms from scratch because technology was their entire value proposition. But these were well-funded bets. They didn’t even build everything from scratch. For example, Oscar partnered with Datavant for clinical data exchange, whereas Ro acquired Workpath for in-home logistics.
Meanwhile, the majority of tech teams choose off-the-shelf software specifically to accelerate time-to-value. Not because they lack ambition, but because rebuilding appointment scheduling from scratch when a $118/month SaaS tool handles it perfectly is a waste of limited runway. The same logic applies to patient portal development — buy the standard layer, build the parts that drive your model.
The question isn’t what’s better in theory. It’s what’s better for where you are right now.
Hidden Costs Associated with Off-the-Shelf Healthcare Software
The sticker price on off-the-shelf healthcare platforms is deceptive. A small practice might see $20,000–$65,000 for implementation and think that’s the number. It’s not even close.
Software cost is only a fraction of the actual cost of ownership. The rest is training, migration, integrations, and the annual support fees that quietly eat your budget every year.
Here’s what the sales deck won’t show you:
Per-provider pricing that doesn’t scale. Tools like RXNT charge $118/month per provider. It’s perfectly manageable for a solo practitioner or a 3-provider clinic. If you add 15-20 providers, you end up paying $28,000+ a year, before even customising anything.
Price hikes are the new normal. SaaS vendors hike prices annually while IT budgets grow only 2.8%. Over 50% of vendor revenue growth now comes from price increases on existing customers, not from acquiring new ones.
Vendor lock-in is by design. Epic uses a proprietary Chronicles database. Oracle Health (formerly Cerner) uses proprietary CCL. Neither is compatible with anything else. Once you’re in, getting out isn’t easy. Data migration alone can cost $20,000–$50,000, and that’s before you factor in retraining your team. Some vendors offer “free” add-on modules that look like savings but are actually lock-in mechanisms; the more modules you use, the more painful it becomes to leave.
The customization ceiling. This is the one that kills startups slowly. Athenahealth pushes centrally controlled updates that interfere with local workflows. DrChrono lags during peak hours and offers limited billing customization. Practice Fusion’s “simple charting” focus means limited advanced features by design. The platform works well until your workflow doesn’t fit its assumptions. You are then either adapting your process to the software or paying for custom integrations, which in turn defeats the purpose of buying it in the first place.
💡 Expert Tip: Ask any SaaS vendor for their price increase history over the last 3 years. If they won’t share it, assume 15–20% annual hikes and factor that into your 5-year TCO. The cheap option in year one is often the expensive option by year three.
Ready to build your custom healthcare software with us? Reach out now – our experts are just one click away.
What Custom Software Development for Healthcare Actually Costs
Building custom software can come across as something easy and enabling. Until you see the costs. These costs aren’t just for the initial development but for everything that comes after.
The build itself. A HIPAA-compliant custom application runs $45,000–$120,000 on average. An MVP with core features on one end, a full-featured platform with integrations on the other. Those numbers assume a competent healthcare app development company that’s built regulated software before — one that knows what healthcare CRM software development actually demands once HIPAA, billing, and patient consent flows enter the picture. If your team is learning HIPAA on the job, expect costs to be 30-40% higher due to mistakes along the way.
Compliance isn’t a one-time cost. Initial HIPAA compliance setup runs $4,000 for a small startup to $150,000+ for a larger operation. However, annual maintenance, including risk assessments, policy updates, employee training, and vendor reviews, adds $10,000–$60,000 every year. And the 2025 Security Rule updates eliminated the “addressable” loophole, mandating encryption, MFA, and annual audits across the board. Compliance is getting harder, not easier.
The talent problem is real. Healthcare software engineers command $147,000–$205,000 in salary. In New York, the average is $192,500. Fully loaded (salary + benefits + equity + overhead), a senior engineer costs $250,000–$350,000 per year. And healthcare tech startup job postings increased 69% year-over-year in 2025, so everyone’s competing for the same talent pool.
Timeline overruns are the norm, not the exception. 70% of healthcare IT projects experience delays, cost overruns, or outright failure. The Standish Group’s 2024 CHAOS report found that only 29% of large custom software projects are delivered successfully. Expect costs to run at least 20% over on any significant build.
Maintenance never stops. Annual maintenance runs 15–20% of the initial development cost. Vulnerability scanning adds $10,000–$30,000 per year. Security patches, compliance updates, server costs, and monitoring aren’t optional. They’re the price of owning your own software.
None of this means building is the wrong choice. It means building is an investment, not a purchase. If you’re going to build, go in with realistic numbers and the right software development partner — one that’s shipped regulated healthcare software before.
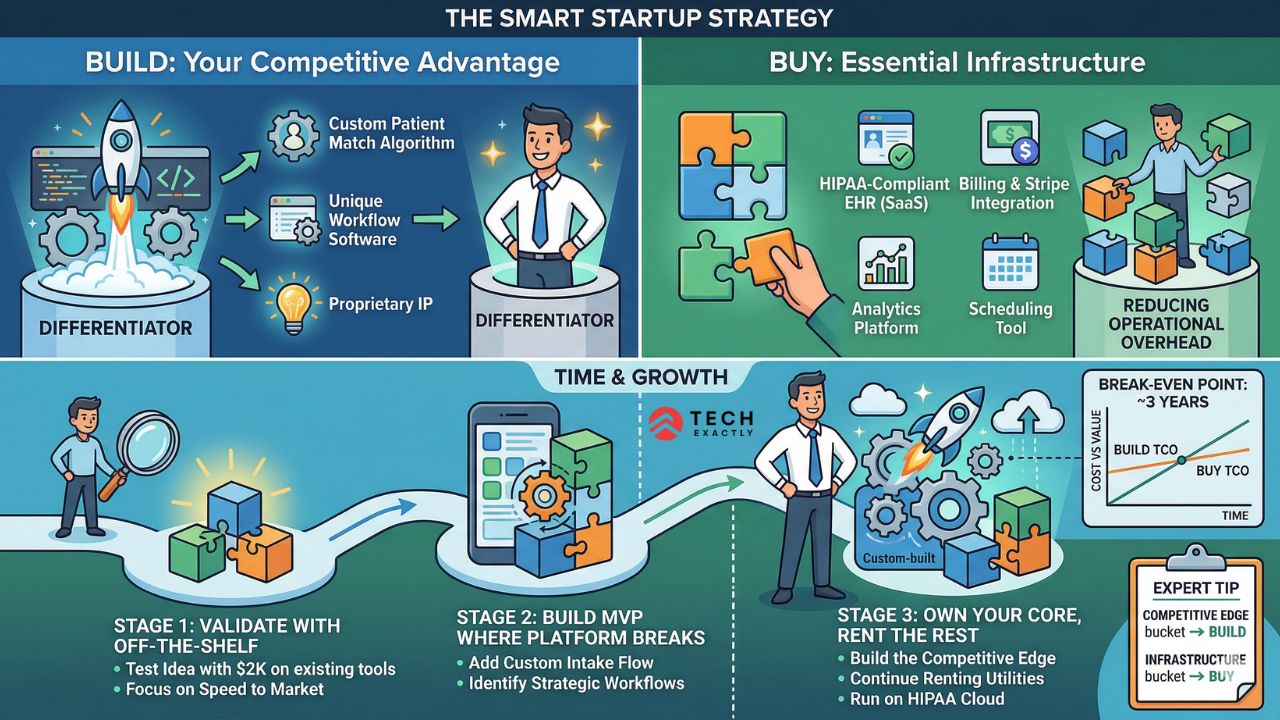
The Hybrid Build vs Buy Approach for Healthcare Startups
The smartest healthcare startups don’t purely build or purely buy. They do both strategically.
Successful health tech companies, from early-stage startups to the billion-dollar players like Oscar Health and Hims & Hers, follow the same pattern. They build custom for what gives them an edge over others and make them different. They buy everything else. Even Oscar partnered with Datavant for clinical data exchange rather than building that piece in-house, saving 25% on that function.
For early-stage startups, small practices, and first-time founders, this plays out in stages:
Stage 1: Validate with off-the-shelf. You have an idea for a healthcare app. Before you spend $50K building it, test the concept using existing tools. You can always spend $5,000 -$2,000 to test a $200/month EHR, a no-code form builder, or even a basic Stripe integration. Healthcare startups using pre-configured compliance environments can market faster than those building from scratch. If the idea doesn’t work, you’ve lost weeks, not your entire seed round.
Stage 2: Build your MVP where the platform breaks. Once you’ve validated the idea, identify the one or two workflows where the off-the-shelf tool is holding you back. Maybe it’s a custom intake flow that Practice Fusion can’t handle, or a patient matching algorithm that no SaaS tool offers. That’s where your custom development budget goes — often built on a clean SaaS development foundation. Not everywhere — just where it matters.
Stage 3: Own your core, rent the rest. As you grow, build, and own the software that IS your competitive advantage. Continue using SaaS for billing, scheduling, and other basic analytics. Basically, all the commodity functions where custom code adds no strategic value. Run it on HIPAA-compliant cloud healthcare computing infrastructure (AWS, Azure, or GCP) and build your application layer on top.
The break-even point? Custom software TCO breaks even with SaaS subscriptions within approximately three years. After that, you are saving money every month while owning an asset that grows in value. Instead of paying for someone else’s platform, which adds costs over time.
💡 Expert Tip: Before you commit to building anything, list every software function your startup needs. Separate them into two buckets: competitive edge and infrastructure. Build the first bucket and buy the second. If everything falls under infrastructure, custom software may not be necessary at this stage, and that’s perfectly fine.
Ready to build your custom healthcare software with us? Reach out now – our experts are just one click away.
How to Decide: A Custom Healthcare Software Decision Framework
So, how do you decide on a custom healthcare software framework? The five questions below will help you make the right decision.
1. Is the software your product, or does it support your product?
If your software is what gives you a competitive edge in the market and is the sole reason why investors bet on your startup, then build it. If it is just the tool your clinical team uses to deliver care, buy it and spend your engineering budget on what actually differentiates you.
2. Do you have product-market fit yet?
If you’re pre-revenue or still iterating on your care model, building custom software is premature optimization. You’ll build the wrong thing. Use off-the-shelf to validate, then build once you know exactly what you need. Startups that validate first build faster, waste less, and end up with a sharper sense of what their healthcare app development cost actually needs to cover.
3. What’s your 5-year TCO, not your year-one cost?
A $200/month SaaS tool looks cheap until you factor in 15–20% annual price hikes, per-user scaling costs, integration fees, and the migration cost when you inevitably outgrow it. Run the 5-year number. Hidden integration and training costs significantly add up on top of a license fee over time.
4. Can your team maintain what you build?
Building is the easy part. What’s difficult is maintaining the processes. Patching, updating for new regulations, and passing security audits every year requires a solid team. If you don’t have the team to maintain custom software long-term, you’ll either hire one (expensive) or let the software degrade (dangerous in healthcare).
5. What happens when you need to scale?
Off-the-shelf platforms scale predictably. You can add users and pay more. Whereas, custom software scales unpredictably. You might have to redesign the database, add infrastructure, or rewrite modules. But custom software scales on your terms, not on a vendor’s pricing model. If you’re planning to grow from 5 providers to 500, the math shifts heavily toward custom.
Healthcare Software Build vs Buy: Common Calls Founders Actually Face
Most healthcare founders face the same questions and dilemmas. It’s more than just building or buying.
Should you build or buy a HIPAA-compliant backend?
For most startups, buy the foundation, build the differentiator.
Managed healthcare PaaS providers, such as Datica, TrueVault, Aptible, provide HIPAA-compliant infrastructure (BAAs included) for $500–$3,000/month.
If you build the same hosting, audit logging, and access controls from scratch on AWS or Azure, you will spend upwards of $40K–$80K. That’s on top of 1–2 dedicated ops hours per week for maintenance.
There’s a big exception, though. If the backend is your product, i.e., you are selling a healthcare developer platform, your only option is to build it. Otherwise, just pick the best available solution.
Build or buy the doctor billing module?
Buy unless you’re a billing-focused startup.
Pre-built RCM modules from AdvancedMD, Kareo, or RXNT cost $99–$300/month per provider and handle CPT codes, ERA processing, and claims scrubbing.
A custom billing module starts at $50K and never stops needing updates as ICD-10 codes, payer rules, and Medicare guidance change quarterly.
The only time custom wins: when your billing is non-standard — value-based care, bundled payments, subscription models — and the SaaS tools can’t represent your contracts.
Built-in forms vs custom HIPAA-compliant intake forms?
Use the platform’s built-in forms for standard intake (name, DOB, insurance, basic history).
Code custom only when the form is part of the clinical product — proprietary screening questionnaires, validated assessment scales, anything that drives downstream automation.
Custom intake forms with conditional logic, FHIR mapping, and HIPAA-compliant storage run $8K–$25K per workflow.
SaaS form modules (Practice Fusion, JotForm Healthcare, Formstack HIPAA) cost $20–$200/month and ship in days.
Don’t pay engineering rates for what’s actually a configuration job.
Time and cost to integrate healthcare software with Epic, Cerner, or Athenahealth?
Plan for $30K–$120K and 4–9 months per EHR.
Epic via the App Orchard program: $2,500–$5,000 program fee plus integration work, with Showroom approval running 3–6 months.
Cerner (now Oracle Health): SMART on FHIR is the path, $40K–$80K typical.
Athenahealth’s Marketplace: faster to onboard, $25K–$60K range.
Add 30–40% if you need bidirectional writes, not just reads.
EHR integration is where most healthcare startup timelines slip — budget for it deliberately, not as an afterthought.
Our EHR integration guide breaks down where the budget actually goes.
Is RXNT at $118/month worth it, or build custom?
For a 1–5 provider practice, RXNT is fine — it’s compliance-ready, ships features, and the math doesn’t justify custom anything.
The break-even shifts at around 12–15 providers.
At $118 × 15 providers × 12 months = $21,240/year, plus surcharges for e-prescribing, billing, and lab integrations that often double the bill.
By year 2–3, you’re at $50K+/year on a tool you don’t own.
That’s when custom modules start to make sense — not a full replacement, but a custom layer on top that handles your highest-volume workflows.
Pre-built revenue cycle module vs custom healthcare RCM?
Buy. Healthcare RCM is a solved problem dominated by AdvancedMD, eClinicalWorks, athenaCollector, and DrChrono.
They handle ERA/EFT, denials management, payer rules, statement generation.
A custom RCM build runs $120K–$400K, takes 9–14 months, and needs continuous updates as CMS publishes new MAC rules.
Unless you’re building a clearinghouse or your business model is revenue cycle (Olive AI, Waystar, Cedar Pay), use a pre-built module.
Build only the patient-facing layer on top — that’s where startups usually have a real edge to capture.
Healthcare Software Compliance Across the US, UK, and Canada
The build-vs-buy framework holds across markets, but the regulatory math underneath shifts. If you’re selling cross-border or starting outside the US, run the numbers per market.
United States
HIPAA, HITECH, and state laws (California’s CCPA/CPRA, New York’s SHIELD Act, Texas Medical Records Privacy Act).
HIPAA setup runs $4K–$150K+, with ongoing costs of $10K–$60K per year.
State breach-notification laws stack on top of federal HIPAA. Multi-state startups need legal review of each market they enter.
United Kingdom
UK GDPR and the Data Protection Act 2018 replace HIPAA’s role.
NHS-facing software requires the NHS Data Security and Protection Toolkit (DSPT).
This involves an annual self-assessment plus an optional independent audit.
Software classified as a medical device needs UKCA marking (which replaced CE marking post-Brexit) and MHRA registration.
UK GDPR fines can go as high as £17.5M or upto 4% of global turnover. That’s significantly higher than HIPAA’s per-violation cap.
Off-the-shelf SaaS sold in the UK should already carry DSPT and UK GDPR coverage. Always verify before signing.
Build-side costs typically add £15K–£60K for proper UK GDPR architecture, including:
- Data residency setup
- DPIA documentation
- Lawful-basis logging
Canada
PIPEDA applies at the federal level, with provincial overlays including:
- Ontario PHIPA
- Alberta HIA
- Quebec Law 25
Quebec Law 25 is the strictest, with breach reporting and consent rules close to GDPR.
SaMD products require a Health Canada Medical Device Licence under SOR/98-282.
Quebec’s Law 25 has significantly increased compliance costs. Most US-built SaaS tools are not Quebec-ready out of the box.
This means custom builds for Quebec markets often run 20–30% higher than US-equivalent budgets.
Plan for data residency requirements as well. Canadian PHI generally needs to stay within Canadian data centres, ruling out many US-only SaaS tools.
The takeaway
A US-centric off-the-shelf tool that costs $200/month at home can become a $2,000/month tool once UK and Canada compliance layers are added — or worse, become unusable.
Multi-market plans tend to push the decision toward custom builds or toward platform vendors that already operate across all three jurisdictions.
Tech Exactly’s medical device software development services and healthcare engineering teams work across the US, UK, and Canada, mapping compliance overhead before any code gets written.
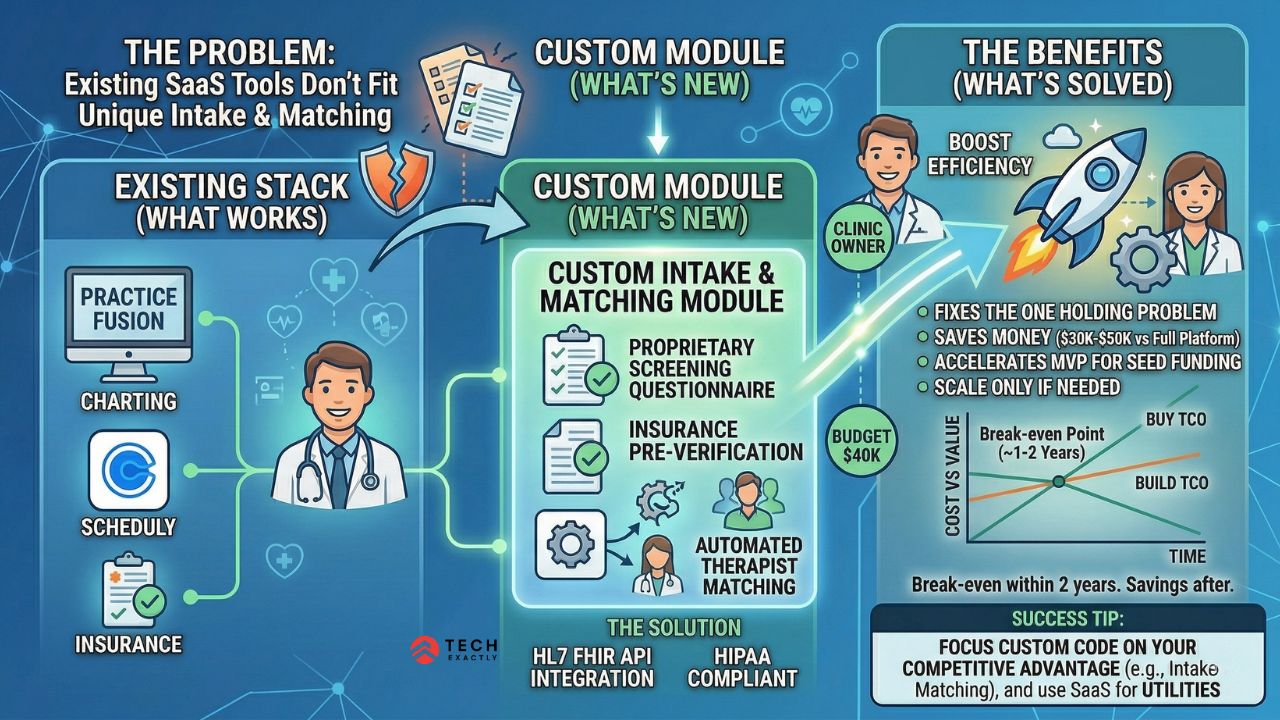
Custom Healthcare Software Development in Action
A first-time founder comes to Tech Exactly with an idea for a mental health platform. They’ve been running a small therapy practice, using Practice Fusion for charting and Calendly for scheduling. It works but to an extent. Their intake process involves a proprietary screening questionnaire, insurance pre-verification, and automated therapist matching based on specialization. None of that fits inside Practice Fusion’s standard forms.
They don’t need a custom EHR. They need a custom intake and matching module that fits easily in their existing system.
That’s a $30,000–$50,000 custom build — closer in scope to our HIPAA-compliant therapy platform case study than a full platform rebuild. It integrates via HL7 FHIR APIs, follows the HIPAA-compliant app playbook, and solves the one problem that was actually holding them back. Everything else stays on their existing stack until and unless they outgrow it.
A small clinic owner with a $40K budget. A founder with seed funding and one shot to get the MVP right. That’s who this approach is built for.
Top Healthcare Software Development Companies for Startups & SMBs
Choosing the right development partner matters as much as the build-vs-buy decision itself. The wrong partner can turn a $60K custom module into a $200K rebuild. Worse, they can miss the compliances entirely, extending your budget and timeline.
The companies below are worth shortlisting for healthcare software development work, especially for early-stage startups, SMBs, and growing companies.
1. Tech Exactly — Healthcare-First Software Development for Startups and SMBs
Tech Exactly is a healthcare app development company built around the realities of startups and SMBs: tight budgets, hard compliance lines, and the pressure to ship without breaking HIPAA, FDA, or EHR timelines.
We work across the US, UK, Canada, and other global markets, with deep coverage of HIPAA, UK GDPR + NHS DSPT, PIPEDA, and IEC 62304 for Software-as-a-Medical-Device (SaMD).
Unlike other companies, we do not treat compliance as an add-on. We scope it in from day one, ensuring we can hit timelines and avoid unnecessary rework later on.
Tech Exactly’s approach is simple. We don’t try to sell custom builds when SaaS is the right call. We open every engagement with a workflow map, identify the one or two pieces that genuinely need custom code, and scope around that.
The result is faster time-to-market and meaningfully lower year-one costs than a full-platform build.
Engagements range from focused module work — custom intake flows, EHR integrations, FHIR mapping layers — through to full platform builds, with most clients landing in the MVP-to-mid-stage range.
Compliance assets we build for include HIPAA risk assessments, BAA-compliant cloud architectures (AWS, Azure, GCP), SOC 2 Type II readiness, ISO 13485 documentation for medical device clients, and DSPT submissions for UK NHS-facing software.
We also handle the more complex tasks that many companies and founders underestimate: security architecture, vulnerability scanning, post-launch maintenance, and yearly compliance audits.
Key strengths:
- Healthcare-first focus: HIPAA, HITECH, UK GDPR + DSPT, PIPEDA, IEC 62304, FDA SaMD pathway, ISO 13485
- EHR integration experience: Epic App Orchard, Cerner / Oracle Health SMART on FHIR, Athenahealth Marketplace, custom HL7 v2 + FHIR interfaces
- Hybrid build-vs-buy delivery: Custom only where it actually moves the business; SaaS layers selected, configured, and integrated where they don’t
- Compliance baked into engineering: Not a QA checklist tacked on at the end
- Flexible engagement models: Fixed-scope MVP, dedicated team, or compliance-only advisory
Get a build-vs-buy assessment for your healthcare startup →
2. ELEKS
A long-running enterprise software firm with a dedicated healthcare practice covering EHR integration, clinical decision support, medical imaging, and HITRUST-aligned delivery.
Strong on complex enterprise systems with real regulatory weight — health systems, payers, and large pharma.
The team size and process maturity tend to make ELEKS a better fit for funded scale-ups and established provider organisations than for seed-stage startups, with discovery and delivery cycles run on the enterprise pattern.
If you need a partner who can stand alongside a hospital IT department, ELEKS is usually on the shortlist.
3. HTD Health
A US-based, healthcare-only product studio that has built one of the more visible build-vs-buy advisory practices in the digital health space.
Often turns up in mid-tier RFPs alongside peer shops, with a portfolio leaning toward clinically complex platforms — care coordination, behavioural health, payer-provider tooling, and value-based care infrastructure.
HTD’s content marketing reads like in-house consulting, which is roughly how they sell.
Strong on product strategy and design-led delivery; less of a fit if you want a pure execution partner who’ll just build to spec.
4. Topflight Apps
A healthcare-focused product agency known for AI-heavy clinical applications, mobile-first telehealth, and a steady stream of healthcare AI thought leadership.
Topflight skews toward founders who want a partner with strong product instincts and AI/ML depth — image recognition, clinical NLP, predictive risk scoring — rather than a pure HIPAA infrastructure builder.
Better fit when AI is the differentiator than when the differentiator is regulatory complexity or deep EHR plumbing.
5. Mindbowser
A healthcare and AI-focused shop with notable depth in FHIR integration, telehealth, and remote patient monitoring platforms.
The portfolio leans toward connected-care plays — wearables, RPM dashboards, digital therapeutics — and the team has built a reputable practice around HL7 v2 to FHIR migrations.
A credible option for founders who want healthcare-specific experience without the enterprise overhead.
6. Arkenea
A healthcare-only firm with a long track record of HIPAA-compliant mobile and web builds for US healthcare clients.
Arkenea is strong on regulatory documentation and standardised compliance deliverables — they tend to produce the kind of audit trail that survives an enterprise security review.
The trade-off: their delivery process favours predictability over speed, which can feel slow if you’re a seed-stage founder iterating on an MVP every two weeks.
Better fit for established providers and mid-market healthcare companies who value process discipline over rapid iteration.
Ready to build your Custom Healthcare Software with us? Reach out now – our experts are just one click away.
Healthcare Software Build vs Buy: FAQ
Anywhere from $45,000 for a focused HIPAA-compliant MVP to $150,000+ for a full-featured platform with integrations. Most early-stage startups and small businesses land in the $45,000–$80,000 range for their first custom build. The final cost really comes down to how complex the product is, the level of compliance required, and how many systems it needs to connect with
A focused custom module (intake, scheduling, patient engagement) takes 3–5 months. A full platform build takes 9–18 months. It’s wise to budget for a 20% timeline overrun, as delays affect 70% healthcare IT projects
You can choose off-the-shelf in the following scenarios: you are pre-revenue or still validating ideas, or software isn't your competitive differentiator, or your budget is under $40K, and you need something real quick within a few weeks. Use off-the-shelf to ship fast and learn, then build custom once you know exactly where the platform is holding you back.
Use off-the-shelf to ship fast and learn, then build custom once you know exactly where the platform is holding you back. The behavioral health software build vs buy decision walks through this in a specific vertical.
Custom software TCO typically breaks even with SaaS subscriptions in approximately 33 months. Subsequently, the cost becomes cheaper month by month. Moreover, now you own the asset instead of renting it.
For anything touching patient data — yes. Healthcare app compliance across HIPAA, GDPR, FDA, and UKCA, HL7 FHIR integration, FDA considerations for clinical software — these aren't things a general-purpose dev shop learns on the fly.
Manas Das, Mobile App Architect at Tech Exactly, has over 9 years of experience leading teams in iOS, Android, and cross-platform development. He specialises in scalable app architecture and GenAI-driven mobile innovation.
