The Real Cost of RPM Software: Per-Patient Pricing, CMS Reimbursement, and When Custom Wins

Key Takeaways
- Off-the-shelf RPM platforms work until they don’t. Most hit a wall around 500 patients — either the per-patient pricing eats your margins, the EHR integration breaks, or you can’t customize clinical workflows without begging their product team.
- Custom RPM software development runs $150,000–$350,000 for a production-ready platform. An MVP with one condition pathway (cardiac or diabetes) can ship in 4–5 months for $80,000–$130,000.
- CMS reimbursement codes (99453, 99454, 99457, 99458) can generate $120–$200 per patient per month. That math changes the entire build-vs-buy equation once you scale past 200 patients.
- The hardest part isn’t the software — it’s device logistics. Getting Bluetooth peripherals into patients’ homes, keeping them charged, and troubleshooting connectivity for 70-year-olds is an operational problem that no platform solves well out of the box.
- AI-driven anomaly detection is moving from “nice-to-have” to “table stakes.” Payers and ACOs are starting to require predictive risk alerts as a condition for RPM program reimbursement.
A health system launches an RPM (Remote Patient Monitoring) pilot with one of the established platforms like Vivify Health, Health Recovery Solutions, or CoachCare. The pilot works fine. 50 patients, heart failure monitoring, with the vendor handling everything. With the readmission numbers dropping, the management gives a go-ahead for a full rollout.
That’s when things start falling apart.
Adding 500 patients means the per-patient-per-month fee increases from a reasonable figure to as much as $15,000–$25,000 a month. There are mapping issues between the platform’s EHR integration and the specific Epic build. Nurses are double-documenting because the RPM dashboard doesn’t feed directly into their clinical notes. The vendor’s product roadmap prioritizes features for larger clients, and the custom workflow your pulmonology department needs is “on the backlog.”
The health system is kind of stuck. They’ve invested 9 months into a platform that solves the pilot but cannot scale with them. Switching vendors will result in re-enrolling every patient, re-training staff, and potentially losing continuity of the data that’s driving their outcomes.
We’ve seen this play out three times in the last year at our healthcare app development company. The conversation always starts the same way: “We need to talk about building our own.”
This guide is for the people having that conversation right now.
The Real Remote Patient Monitoring Software Landscape in 2026
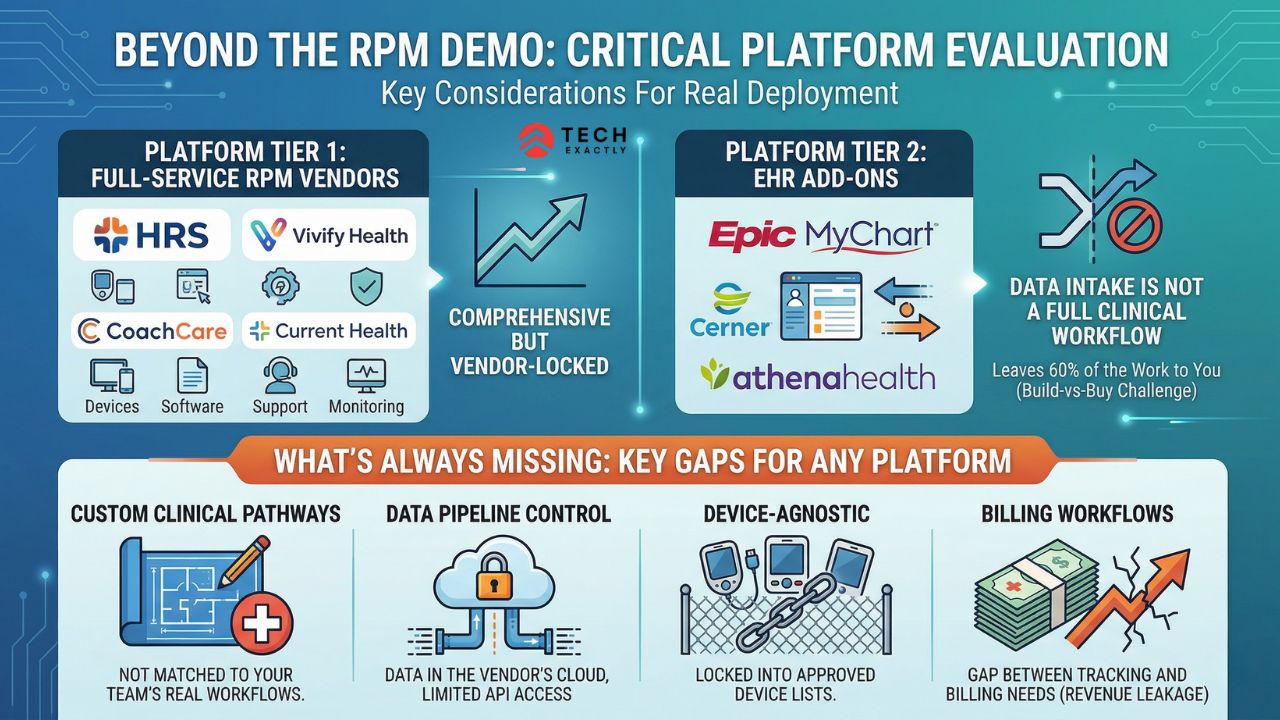
Skip the vendor marketing for a minute. Here’s what the platform options actually look like when you’re evaluating them for a real deployment and not just a demo.
Platform Tier 1: Full-Service RPM Vendors
These companies sell the whole package: devices, software, patient enrollment support, clinical monitoring services.
| Platform | Strengths | Where It Breaks | Pricing Model |
|---|---|---|---|
| Health Recovery Solutions (HRS) | Strong chronic disease pathways, good patient engagement tools, dedicated clinical team option | Limited EHR customization beyond Epic/Cerner basics. Custom analytics requires the team’s involvement. | Per-patient/month ($50–$100+). Volume discounts for above 300 patients. |
| Vivify Health (Optum) | Enterprise scale, Optum/UHG backing, robust data analytics | Post-acquisition integration friction. Smaller clients report slower support response. Locked into the Optum ecosystem. | Enterprise contract. Minimum commitments. |
| CoachCare | Good for private practices, lower entry point, white-label option | Thinner clinical pathway library. Device ecosystem is narrower. Integration depth beyond basic HL7 is limited. | Per-patient/month ($35–$75). Lower volume requirements. |
| Rimidi | Strong for diabetes and cardiometabolic. Clinical decision support built in. | Narrow condition focus. Not ideal for multi-specialty RPM programs. | Custom pricing. |
| Current Health (Best Buy Health) | FDA-cleared wearable (biosensor patch), continuous monitoring | Consumer retail backing creates uncertainty about long-term healthcare commitment. Limited clinical workflow customization. | Device + platform fee. |
Platform Tier 2: RPM-Capable EHR Add-ons
Epic’s MyChart integrates RPM device data. Cerner (now Oracle Health) has remote monitoring modules. Athenahealth offers basic RPM workflows.
You might think you have EHR and only need to add RPM.
But the reality is different. They only handle the data intake.
These modules handle data intake but rarely deliver the clinical workflow layer. You still need someone to build the alert logic, escalation paths, patient communication sequences, and device management. This is the same build-vs-buy challenge that comes up across every healthcare software category. They solve 40% of the RPM problem and leave you to figure out the rest.
What None of These Platforms Give You
- Condition-specific clinical pathways you designed. Every vendor sells pre-built protocols. None of them match how your clinical team actually operates. The gap between “close enough” and “exactly right” is where patient safety lives.
- Full control over the data pipeline. Your RPM data is in someone else’s cloud. Extracting it for your own analytics, combining it with claims data, or feeding it into your population health platform requires their API. This has rate limits, costs extra, and does not expose everything.
- Device-agnostic architecture. Most platforms lock you into their approved device list. When a better blood pressure cuff hits the market or your cardiologists want a specific ECG patch, you are stuck filing a feature request and waiting.
- Custom billing workflows. CMS reimbursement for RPM needs accurate time tracking and documentation. Every platform handles this in a different way, and none of them map perfectly to your billing team’s existing workflow. There’s a big difference between what the platform tracks and what your billers need to submit claims, and is a big area of revenue leakage.
Let's Start Your Project Today
Ready to build your Remote Patient Monitoring Software with us? Reach out now – our experts are just one click away.
Remote Patient Monitoring Software Pricing: The Numbers Nobody Publishes
Vendors don’t put pricing on their websites for a reason. It varies significantly by patient volume, contract length, and how hard you negotiate. Here is what we have seen across real engagements.
SaaS Platform Costs (Off-the-Shelf)
| Scale | Monthly Platform Cost | Per-Patient/Month | Annual Total |
|---|---|---|---|
| Pilot (50 patients) | $2,500–$5,000 | $50–$100 | $30,000–$60,000 |
| Mid-scale (300 patients) | $12,000–$22,000 | $40–$75 | $144,000–$264,000 |
| Full deployment (1,000 patients) | $35,000–$65,000 | $35–$65 | $420,000–$780,000 |
| Enterprise (3,000+ patients) | $80,000–$150,000 | $27–$50 | $960,000–$1,800,000 |
Further, add device costs, like $50–$200 per patient for an initial kit: BP cuff, pulse oximeter, scale, tablet, and connectivity costs ($5–$15/month per patient for cellular-enabled devices).
Custom Development Costs
| Phase | Scope | Cost Range | Timeline |
|---|---|---|---|
| MVP | Single condition pathway (e.g., cardiac), device integration (3–4 peripherals), patient app, clinical dashboard, basic alerts, HIPAA-compliant cloud | $80,000–$130,000 | 4–5 months |
| Phase 2 | Multi-condition support, automated escalation logic, CMS billing integration (CPT code time tracking), EHR integration (Epic/Cerner FHIR APIs), reporting dashboard | $60,000–$120,000 | 3–4 months |
| Full Platform | AI-driven risk stratification, multi-site deployment, device management portal, patient self-enrollment, white-label capabilities, API for third-party integrations | $50,000–$100,000 | 2–3 months |
| Total | Production-ready RPM platform | $190,000–$350,000 | 9–12 months |
The Crossover Point
Here’s where the math gets interesting.
At 200 patients, off-the-shelf costs roughly $8,000–$15,000/month ($96,000–$180,000/year). Custom platform maintenance runs $3,000–$6,000/month after the initial build. You’ve already recovered the development investment within 18–24 months.
At 500 patients, off-the-shelf runs $20,000–$37,000/month. Your custom platform’s marginal cost per additional patient is near zero. There is only cloud compute, which scales linearly at pennies per patient.
At 1,000 patients, it’s not even close. You are paying $420,000–$780,000/year for a platform you don’t control, or you are running your own at $50,000–$80,000/year in infrastructure and maintenance.
The breakeven for custom development is typically 200–400 active patients, depending on your vendor’s pricing and how aggressively you negotiated the SaaS contract.
CMS Reimbursement: The Revenue Engine That Justifies Everything
CMS introduced RPM-specific billing codes in 2018 and has expanded coverage consistently since. Here’s what you can bill in 2026:
| CPT Code | What It Covers | Reimbursement | Frequency |
|---|---|---|---|
| 99453 | Initial patient setup and education on RPM devices | ~$19 | Once per patient |
| 99454 | Device supply and daily data transmission (minimum 16 days/month) | ~$55 | Monthly |
| 99457 | First 20 minutes of clinical staff time reviewing RPM data and communicating with patient | ~$50 | Monthly |
| 99458 | Each additional 20 minutes of clinical staff time | ~$42 | Monthly (up to 2 additional) |
| 99091 | Collection and interpretation of physiologic data (minimum 30 minutes) | ~$56 | Monthly |
Revenue Per Patient Per Month
Conservative scenario (99454 + 99457 only): ~$105/patient/month
Moderate scenario (99454 + 99457 + one 99458): ~$147/patient/month
Full capture (99453 setup + 99454 + 99457 + two 99458 + 99091): ~$205/patient/month in the first month, ~$203/month ongoing
What This Means for Your Build Decision
| Patients Enrolled | Monthly Revenue (moderate) | Annual Revenue | Custom Dev ROI |
|---|---|---|---|
| 100 | $14,700 | $176,400 | Pays for MVP in ~6 months |
| 300 | $44,100 | $529,200 | Full platform cost recovered in ~8 months |
| 500 | $73,500 | $882,000 | Net positive even after ongoing maintenance |
| 1,000 | $147,000 | $1,764,000 | You’re running a profit center, not a cost center |
The catch: you can only tap this revenue if your software can document time accurately, flag the 16-day transmission threshold per patient, and generate audit-ready reports. Almost all SaaS platforms handle this, but the ones that do it well charge accordingly. Building this into your custom platform is a $15,000–$25,000 development effort, and it pays for itself with 20 patients.
What Custom Remote Patient Monitoring Software Actually Requires
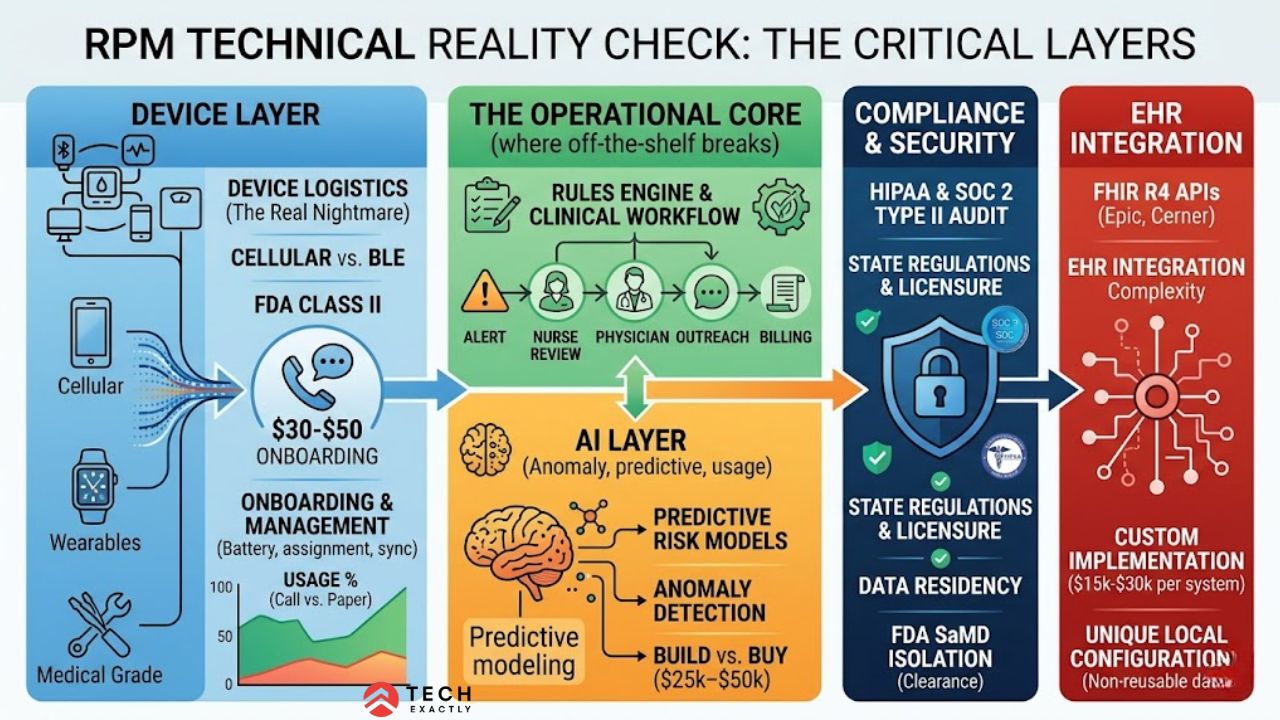
Not a feature list but a technical reality check.
The Device Layer (The Part Everyone Underestimates)
RPM software is only as good as the data fed to it. That means devices and that’s where RPM programs start to break down.
What you need to support:
- Bluetooth Low Energy (BLE) peripherals: blood pressure cuffs (Omron, A&D Medical), pulse oximeters (Masimo, Nonin), weight scales (Withings, BodyTrace), glucose meters (OneTouch Verio, Dexcom CGM).
- Cellular-enabled devices: for patients without smartphones or reliable Wi-Fi. BodyTrace and Vivify offer cellular-embedded devices, but they keep you stuck in their ecosystem.
- Wearables: Apple Watch (HealthKit), Fitbit/Google (Health Connect API), Garmin, Biobeat for continuous vitals. Integrating these into a unified data pipeline is one of the harder parts of AI-driven app development.
- Medical-grade vs. consumer-grade: FDA-cleared devices (Class II) are required for clinical decision-making. Consumer wearables are supplementary only.
The operational nightmare nobody talks about:
Getting a Bluetooth blood pressure cuff paired with a 72-year-old COPD patient’s Android phone, in their home, via a phone call with a support tech, is the real challenge. Neither the software architecture nor the FHIR integration.
Device logistics is a world of its own. Shipping, asset tracking, patient onboarding calls, replacement workflows for lost or broken devices, battery management, and connectivity troubleshooting. If you are building custom, you need to build or integrate a device management module that tracks which device is assigned to which patient, last sync time, battery status, and firmware version.
💡 Expert Tip: Consider a budget of $30–$50 per patient for device onboarding support (phone-based setup assistance). The clinical outcomes data are very clear. Programs with dedicated device onboarding see 85–92% consistent device usage. Programs that ship devices with a printed instruction sheet see 40–55%. That delta is everything.
The Clinical Workflow Layer
This is the layer where off-the-shelf platforms break down and custom development earns its cost.
Alert logic that reflects how your team actually works:
Every clinical team handles RPM alerts in a different way. A heart failure program might escalate a weight gain of 3+ lbs in 48 hours to a nurse immediately. On the contrary, a hypertension program routes elevated BP readings to a queue for next-day review. Your software needs configurable alert rules and not just threshold-based triggers, but multi-variable logic that accounts for patient baselines, medication changes, and known patterns.
This is not a settings page. It’s is a rules engine. Building a flexible, clinician-configurable rules engine is typically $20,000–$35,000 of development effort and is the single feature that most justifies going custom.
Escalation paths:
Alert → nurse review → physician notification → patient outreach → documentation. Every step needs to be logged with timestamps (for CMS billing), and the entire chain needs to be auditable. If your escalation logic stays in email threads and sticky notes, you are leaving reimbursement on the table and exposing yourself to liability.
The AI Layer (No Longer Optional)
Three years ago, AI in RPM was a mere pitch deck feature. Now payers and ACOs are asking for it specifically.
What’s actually viable in 2026:
- Anomaly detection: Flag readings that move away from a patient’s established baseline, not just static thresholds. A blood pressure of 145/92 might be alarming for one patient and completely normal for another. Baseline-adjusted alerting reduces false positives by 40–60%.
- Predictive hospitalization risk: Models trained on vitals trends, medication adherence, and social determinants that flag patients are likely to decompensate in the next 7–14 days. Several published models achieve AUC 0.78–0.85 for 30-day readmission prediction.
- Engagement prediction: Identify patients whose device usage patterns suggest they’re about to drop off, and trigger proactive outreach before they disengage entirely.
What’s still hype:
- Fully autonomous clinical decision-making (no payer accepts this yet)
- Natural language processing for patient-reported symptoms at scale (accuracy isn’t reliable enough for clinical action)
- Federated learning across health systems (technically possible, practically no one is doing it)
Building the AI layer into a custom RPM platform adds $25,000–$50,000 to development costs. If you use pre-trained models from cloud providers like AWS HealthLake, Google Cloud Healthcare API, and Azure Health Data Services, it can reduce the cost by half. However, you trade customization for speed. If you are evaluating how AI fits into broader healthcare product strategy, our guide to AI in healthcare app development covers the landscape beyond RPM.
Compliance and Security
HIPAA compliance is the baseline, not the end. Your RPM platform also needs:
- FDA SaMD classification awareness: If your software’s algorithms influence clinical decisions (e.g., “this patient’s cardiac risk is elevated”), it may qualify as Software as a Medical Device. Most of the RPM platforms are exempted under FDA enforcement discretion, however that is a policy choice that could change. You need to build your system so the AI layer can be isolated and submitted for clearance if regulations shift.
- SOC 2 Type II: Not legally required, but health systems increasingly demand it from technology vendors. A penetration test is a prerequisite. Plan for the full audit ($15,000–$30,000) and build controls into the platform from day one.
- State-level telehealth regulations: RPM reimbursement and licensure requirements vary by state. Your platform needs to handle multi-state provider licensing validation if you’re deploying across state lines. Similar challenges apply to telemedicine app development.
- Data residency: Some health systems require that patient data remain within specific geographic regions. Your cloud architecture needs to accommodate this.
EHR Integration: Where the Real Complexity Lives
You’ll need to integrate with at least one EHR system. Here’s what that actually involves:
FHIR R4 APIs are the standard, and both Epic and Cerner/Oracle Health expose them. The good news is that you can read patient demographics, write clinical observations, and create care plans through standardized endpoints. The bad news is that every health system’s Epic instance is configured differently. The same FHIR endpoint at Hospital A returns data structured differently than Hospital B because of custom extensions, local code sets, and configuration choices made during their implementation.
Consider a budget of $15,000–$30,000 per EHR integration, and don’t expect the first one to be reusable without modification for the second.
Let's Start Your Project Today
Ready to build your Remote Patient Monitoring Software with us? Reach out now – our experts are just one click away.
When Custom RPM Software Development Makes Sense
Not every organization should build custom. Here’s the honest decision framework, which can help you:
Build custom if:
- You are monitoring 300+ patients and the SaaS cost is not sustainable.
- Your clinical workflows are very different that no vendor’s pre-built pathways fit without significant workarounds
- You want to own the patient data pipeline for your own analytics, quality reporting, or research. RPM is a strategic revenue line, not a pilot project.
- You are investing in it as infrastructure
- You need to integrate heavily with your EHR in ways the vendor’s standard integration doesn’t support
Stay on a SaaS platform if:
- You have under 200 patients and don’t have a clear growth projection
- Your RPM program is one condition, one site, standard protocol
- You don’t have internal technical leadership to manage a custom platform, though a software development partner can fill that gap
- You need to launch within 60 days (custom can’t match vendor deployment speed for v1)
The hybrid path:
Some organizations start with a SaaS platform, use it for 12–18 months to learn and understand what works, and then build custom software using the learnings, including all the workflow gaps the vendor couldn’t fill. This is actually a smart approach. You’re paying for education, and the SaaS period generates the requirements spec for your custom build.
How to Choose a Remote Patient Monitoring Software Development Partner

Skip the firms that list “RPM” as one of 47 healthcare capabilities on their services page. You want a team that can answer these questions without checking with their presales department:
- “Walk me through a FHIR R4 integration you’ve done with Epic. What broke?” If they have done it, they will have a specific answer about custom extensions, token expiration, or sandbox vs. production differences. If they have not, they will give you a generic answer about standards compliance.
- “How do you handle BLE device pairing failures for elderly patients?” This suggests that they have actually deployed RPM in the field or just built the software. The device layer is where experience matters most.
- “What’s your approach to CMS billing documentation within the RPM workflow?” Most important is how they track the 20-minute clinical time windows for CPT 99457/99458? How do they flag patients below the 16-day data transmission threshold for 99454? If they look confused, they haven’t built billing-aware RPM software.
- “Show me how your alert escalation engine is configured.” You want to see a rulebook, not hardcoded thresholds. Ask them to show you how a clinician would modify an alert rule without involving a developer.
At Tech Exactly, we have built and re-engineered healthcare platforms that outgrew their first version. Our work spans EHR integrations, regulatory-compliant architectures, and patient-facing applications, which is the full stack that a production RPM platform requires.
The Decision You're Actually Making
If RPM is a checkbox, something your ACO contract requires, something you are piloting to stay relevant, proceed to buy a platform, enroll 50 patients, and move on. The vendor will handle everything, and the cost is manageable at the pilot scale.
If RPM is infrastructure, like a permanent part of how you deliver care, a revenue line you are scaling, a data source feeding your population health strategy, then at some point, you’ll outgrow every vendor. The question is whether you build before or after reaching the limit..
The organizations we work with usually come to us after. They’ve learned enough from the vendor to know exactly what they need. They have 12 months of clinical data proving the model works. And they’re ready to own it.
If that sounds familiar, let’s talk. We’ll scope it with you, whether that’s a custom web application, a native mobile platform, or both. We will show you where the real costs hide, and be straight about whether custom development actually makes sense for your situation. Sometimes it doesn’t, and we’ll tell you that too.
Ready to Get Started?
Get a free quote and see what we can do for you.
FAQs on Remote Patient Monitoring Software
A minimum viable product, which is focused on a single condition like cardiac, diabetes, or COPD, costs between $80,000 and $130,000 and can be developed within 4–5 months. A multicondition platform having AI-driven alerts, CMS billing integration, and EHR connectivity costs around $190,000 to $350,000 and takes 9–12 months. Support and maintenance activities account for 15–20% of the initial build cost annually.
An RPM app is the patient-facing thing that is used by the patient to view readings, communicate with their care team, and receive alerts. RPM software is the entire platform that has device management, a clinical dashboard, an alert engine, billing documentation, EHR integration, analytics, and the patient app. Building just the app is a small component of the full software cost.
Yes, you can use FHIR R4 APIs. Both systems provide standard points to read patient data and write clinical observations. But, each health system’s EHR instance is uniquely configured, which includes custom extensions, local code sets, and distinct workflows. These require tailored mapping and testing for every integration. Budget approximately $15,000–$30,000 per EHR integration.
Through CPT codes like 99453 for initial setup, 99454 for device supply and daily transmission, 99457 for the first 20 minutes of clinical review, 99458 for additional 20-minute increments, and 99091 for data interpretation. At moderate utilization, you can bill about $147/patient/month. Your RPM software needs to track clinical time accurately and flag the 16-day minimum data transmission requirement per patient to ensure compliant billing.
The critical point is typically 200–400 active patients. Below this, the SaaS platforms are more cost-effective and faster for deployment. Above this, the per-patient pricing of SaaS platforms multiplies faster than the maintenance cost of a custom-built platform. Some of the other signs are when your clinical workflows don't fit vendor templates, or you need deep EHR integration beyond standard connectors, or you want full ownership of the patient data pipeline for analytics and research.
At the very least, you need to have Bluetooth blood pressure cuffs, pulse oximeters, weight scales, and glucose meters. For cardiac programs, you require ECG patches. For respiratory programs, you need spirometers. The platform should be able to support both BLE (Bluetooth Low Energy) peripherals paired with patient smartphones and cellular-enabled devices for patients without smartphones. Device-agnostic architecture is most important as you don't want your clinical program fixed to a single device manufacturer.
Pallabi Mahanta, Senior Content Writer at Tech Exactly, has over 5 years of experience in crafting marketing content strategies across FinTech, MedTech, and emerging technologies. She bridges complex ideas with clear, impactful storytelling.
