How We Delivered a HIPAA-Compliant Online Therapy Platform in New York

Key Takeaways:
1. HIPAA violations are costly and rising; healthcare data breaches averaged $10.93 million in 2023, the highest across industries for the 13th consecutive year. (Source: IBM)
2. In 2023 alone, 725 data breaches were reported, affecting more than 133 million records
3. HIPAA penalties are tiered, and fines range from $100 per violation for unknowing violations to $50,000 per violation for willful neglect, with annual caps reaching $1.9 million per violation category.
4. Mental health data carries the highest breach risk valued at up to $1,000 per record on the dark web compared to $1 for a stolen credit card, making therapy platforms a disproportionately high-value target. (Forbes)
When a mental healthcare practice in New York City came to us seeking to expand online, the first question they asked was about features: video sessions, booking, and therapist matching. The first question we asked was about compliance.
That moment captures everything that matters about building online telemedicine platforms for mental health. The product decisions are secondary. The compliance architecture is the product. Get it wrong, and you’re not just facing a failed launch; you’re looking at HIPAA violation examples that can cost anywhere from $100 to $50,000 per violation, per category, per year.
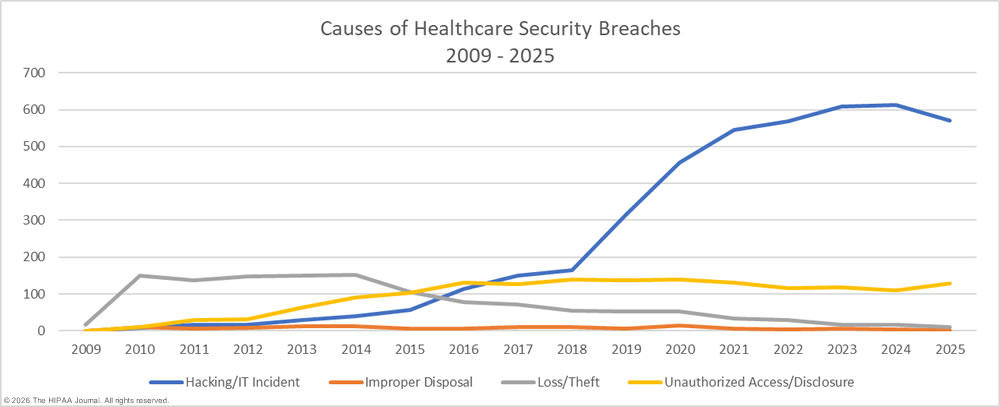
Image Source
This is the story of how we built a HIPAA compliant app development project from scratch for a New York-based therapy platform.
What the challenges were,
how we solved them, and
what every healthcare founder needs to understand before writing a single line of code.
As per Markets and Markets, the global digital health market is projected to reach USD 573.53 billion by 2030, and healthcare startups in New York City are at the centre of that growth. But growth without compliance infrastructure is a liability, not an opportunity. Here’s how to build it right.
HIPAA: What Does It Stand For and Why Does It Define Every Decision in Healthcare App Development?
Before getting into architecture, let’s establish the foundation. Because we’ve seen too many healthcare founders treat HIPAA as a legal afterthought rather than a technical requirement.
HIPAA what does it stand for? The Health Insurance Portability and Accountability Act, signed into law in 1996, establishes the national standard for protecting sensitive patient health information. For any platform handling Protected Health Information (PHI), which includes anything from a patient’s name linked to their diagnosis, to session notes, to appointment records, HIPAA compliance is the law.
HIPAA compliance operates across three rules that directly affect how you architect a healthcare application:
The Privacy Rule: Governs who can access PHI, under what conditions, and requires patients to be informed of their rights.
The Security Rule: Mandates specific technical, administrative, and physical safeguards for electronic PHI (ePHI) encryption, access controls, and audit logs.
The Breach Notification Rule: Requires covered entities to notify patients and HHS within 60 days of a PHI breach.
Understanding HIPAA violation examples makes the stakes concrete. In 2023, a mental health app was fined $7.1 million for sharing patient data with third-party platforms without authorization. A major hospital network paid $6.8 million after a ransomware attack exposed patient records. These aren’t edge cases; they’re the predictable outcome of building healthcare products without compliance at the architectural level.
For healthcare mobile app development services, this means every database schema decision, every third-party integration, every API design, and every user authentication flow is a compliance decision, not just an engineering one.
Related reading → Healthcare App Development in 2026: What Actually Goes Into Building a Compliant Product
The New York Therapy Platform: What the Client Actually Needed
Our client required a secure web application to provide mental health therapy so that patients and therapists situated anywhere in NYC could get healthcare quickly and easily. They wanted to expand their therapy practice online, connecting patients with top therapists in New York City through a single, accessible platform.
The three variables they prioritized were convenience, accessibility, and security in that order. Our job, as their healthcare mobile app development company, was to ensure those three variables were delivered without ever compromising the fourth: compliance.
The platform needed to support:
Secure audio and video counselling sessions connecting patients with therapists across NYC.
A therapist discovery and matching system allowing patients to find the right practitioner.
Patient data management that kept all PHI encrypted, access-controlled, and auditable.
A seamless booking and scheduling system that didn’t create compliance gaps at the appointment layer.
What the client initially underestimated, as most healthcare startups in New York City do, was how deeply compliance requirements would shape every one of these features. The video system couldn’t just use any WebRTC provider. The booking system couldn’t store data in a standard relational database without row-level access controls. The therapist profiles couldn’t be indexed publicly if they contained patient-linked information.
Compliance wasn’t a filter applied at the end. It was the architecture from which everything else was derived.
▶️You might like reading How to Build a HIPAA-Compliant App
What HIPAA-Compliant App Development Actually Looks Like in Practice
This is the section most compliance guides skip. They tell you what HIPAA requires, but not how that translates into technical decisions. Here’s the breakdown of how we approached HIPAA compliant app development for this platform.
Encrypted Data at Rest and in Transit
Every piece of patient data: session notes, appointment history, therapist communications, and payment records was encrypted using AES-256 at rest and TLS 1.2+ in transit. The encryption key management strategy determines whether this protection is meaningful or cosmetic. We implemented a dedicated key management service with tenant-level key isolation, meaning no patient’s data could ever be decrypted using another patient’s credentials.
Role-Based Access Controls
Not everyone on the platform needs to see everything. We implemented granular role-based access:
Patients could access only their own records, session history, and assigned therapist information.
Therapists could access only the patient records of their active and past clients, not the broader patient database.
Platform administrators had audit-level access with full logging of every data access event.
Business Associate Agreements Across Every Integration
Every third-party service that touched PHI: the video conferencing provider, the cloud hosting layer, and the email service for appointment reminders required a signed Business Associate Agreement (BAA) before integration. This is one of the most common gaps in telehealth platforms HIPAA compliant builds. Founders sign a BAA with their cloud provider and assume they’re covered. They’re not because every sub-processor in your stack needs its own agreement.
Audit Logging and Incident Response
Every data access event, every login, every failed authentication attempt, and every PHI modification was logged to an immutable audit trail. This isn’t just a HIPAA requirement; it’s the mechanism that allows you to detect, investigate, and respond to potential breaches within the 60-day notification window the Breach Notification Rule requires.
💡Insider Tip from Tech Exactly: The most commonly missed HIPAA requirement in telehealth builds is the audit log for failed access attempts( not just successful ones). Most teams log what users accessed. Far fewer log what they tried to access and were denied. Regulators look at both. Build your audit logging to capture the full access attempt lifecycle from day one, not just the successful reads.
Related reading → How Healthcare Startups Can Build Regulatory-Compliant Apps Without Slowing Innovation
EHR Health Integration: Why It’s Non-Negotiable for Serious Telehealth Platforms
One of the most significant architectural decisions in building HIPAA-compliant telehealth platforms for a clinical setting is how and whether to integrate with EHR health systems. For a therapy platform, this question is about clinical continuity: can a therapist access a patient’s prior treatment history, medication records, or referral notes from other providers?
EHR systems examples that are commonly integrated into telehealth platforms include Epic, Cerner, athenahealth, and SimplePractice. For behavioural health specifically, platforms like TheraNest and TheraPlatform are purpose-built with EHR health functionality included.
The integration standard in 2026 is FHIR R4 (Fast Healthcare Interoperability Resources), which structures clinical data into discrete, queryable resources rather than requiring full record exports. For our New York therapy client, we designed the EHR integration layer to pull only the specific FHIR resources relevant to each therapist’s session context, not a full chart dump that would create unnecessary PHI exposure.
EHR System | Best For | FHIR Support | HIPAA BAA Available |
Large health systems, hospital networks | Full FHIR R4 | Yes | |
Mid-to-large health systems | Full FHIR R4 | Yes | |
Outpatient practices, SMB clinics | FHIR R4 | Yes | |
Solo/small therapy practices | Partial | Yes | |
Behavioural health, mental health practices | Partial | Yes |
For healthcare startups in New York City building telehealth from scratch, the decision isn’t always which EHR to integrate with. Rather, the question is whether to build lightweight internal EHR health record management within the platform itself, or to build integrations with existing systems your therapist network already uses. For this client, we built both a lightweight internal session note and record system, with an integration layer designed for future EHR connectivity as the practice scaled.
Related reading → The Future of AI in Healthcare Apps: From Diagnostics to Automation
Why the UK and USA Both Need HIPAA-Grade Architecture, Even When Only One Applies
If you’re building a Healthcare App Development Company in USA context, the compliance framework is HIPAA. If you’re operating as a Healthcare App Development Company in UK, the primary frameworks are UK GDPR and the Data Security and Protection (DSP) toolkit for NHS-connected services. But here’s what experienced telemedicine software companies know: the technical architecture that satisfies HIPAA also satisfies most of UK GDPR’s requirements for health data.
Both frameworks require:
Encryption of health data at rest and in transit.
Strict access controls with documented user permission levels.
Audit logging of all data access events.
Data minimization, only collecting and processing the PHI strictly necessary for the stated purpose.
Documented incident response and breach notification procedures.
Building to HIPAA standards from day one means a Healthcare App Development Company in UK engaging US patients, or a US platform expanding to UK markets, doesn’t need to rebuild its security architecture. The foundations are compatible. The legal documentation layer (BAAs vs. Data Processing Agreements) differs, but the technical safeguards are largely aligned.
For healthcare mobile app development services targeting both markets, this is the most efficient path: build to the stricter standard first, then layer the jurisdiction-specific legal documentation on top.
Related reading → How SMBs Can Integrate AI into Existing Software Systems
The Feature Architecture That Made the Platform Work for Patients and Therapists
Beyond compliance, the platform had to actually work intuitively, reliably, and at scale for a New York City user base that has exceptionally high expectations for digital product quality. Here’s how the core feature architecture came together.
Therapist Discovery and Matching
Patients could search and filter therapists by speciality, availability, session format (audio-only or video), and insurance compatibility. The matching layer was built to surface relevant therapists without exposing PHI in the search index, a detail that most consumer-facing health platforms miss entirely.
One-Click Audio and Video Sessions
The platform connected patients with top therapists in NYC with a single click via audio and video chats. The video infrastructure was built on a HIPAA-compliant WebRTC provider with end-to-end encryption, a virtual waiting room architecture that prevented session data from being accessible to non-participants, and automatic session recording controls that required explicit patient consent before activation.
Secure Messaging Between Sessions
Between live sessions, patients and therapists could communicate through an encrypted asynchronous messaging system, purpose-built to keep all communications within the platform’s compliant environment rather than defaulting to standard email or SMS, neither of which is inherently HIPAA-compliant.
All message content was encrypted at the application layer before storage.
Message retention policies were configurable by practice and aligned with state-specific record retention requirements.
Therapists received no-reply notifications via standard email, with the actual content remaining inside the secure platform.
Appointment Scheduling and Automated Reminders
The booking system is integrated with therapist calendars while keeping appointment data, which is PHI when linked to a patient identity and health context within the platform’s compliant data environment. Automated reminders were sent via HIPAA-compliant communication channels with opt-in consent captured during onboarding.
→ Read the full case study: HIPAA-Compliant Website for Therapy
What Every Healthcare Founder Needs to Know Before Starting a Telehealth Build
Whether you’re building online telemedicine platforms for mental health, primary care, or specialist consultations, the lessons from this project apply across the board. Here’s what we’d tell every founder at the start of an engagement.
Compliance is architecture. The most expensive mistake in HIPAA compliant app development is treating compliance as something you add at the end. Every database design, every integration decision, every user flow needs to be evaluated through a compliance lens from the first design sprint.
Your BAA coverage needs to extend to every vendor in your stack. Not just your cloud provider. Your video provider, your email service, your analytics platform, your logging infrastructure if it touches PHI, it needs a BAA. Most telemedicine software companies have these available on request. If a vendor can’t or won’t provide one, they can’t be in your stack.
Data minimization is a feature, not a limitation. Building systems that collect and process only the PHI strictly necessary for each function makes your platform faster, cheaper to operate, and more defensible in an audit. It also reduces your breach surface area as you can’t leak data you never collected.
Start your compliance documentation before your first line of code.
Engage a HIPAA compliance consultant alongside your development team, not separately from it.
Test your audit logging and incident response procedures before launch, not after a breach forces the issue.
Related reading → Generative AI in Healthcare: Use Cases, Benefits & What Founders Need to Know
Working With the Right Healthcare Mobile App Development Company
The difference between a healthcare mobile app development company that can deliver a compliant telehealth platform and one that can’t is rarely about technical capability. It’s about whether compliance is embedded in their development process or treated as a client’s problem.
When evaluating a Healthcare App Development Company in USA or a Healthcare App Development Company in UK for a telehealth build, ask these questions before the first proposal:
Have you delivered HIPAA-compliant builds before, and can you walk me through the specific compliance decisions you made?
Do you have a standard BAA review process for third-party integrations?
How do you handle compliance documentation? Is it generated retroactively or maintained throughout development?
What does your audit logging architecture look like for a telehealth platform?
The answers tell you whether you’re working with a team that has genuinely built in this space or one that is learning on your project.
At Tech Exactly, our healthcare mobile app development services are built around compliance-first engineering. Every healthcare engagement starts with a compliance architecture review before we scope the technical build. If you’re building a telehealth platform and want a software development partner who treats HIPAA compliance as a product requirement, you can connect with us to know more or write to us at info@techexactly.com.
Let's Start Your Project Today
Ready to build your App with us? Reach out now – our experts are just one click away.
Frequently Asked Questions
HIPAA what does it stand for? It is the Health Insurance Portability and Accountability Act. For app development, HIPAA compliance requires:
- Encryption: All PHI must be encrypted at rest (AES-256) and in transit (TLS 1.2+).
- Access controls: Role-based permissions ensure each user accesses only the PHI their role requires.
- Audit logging: A complete, immutable log of every PHI access, modification, and failed access attempt.
- Business Associate Agreements: Signed BAAs with every third-party vendor that processes PHI: cloud providers, video platforms, email services, and analytics tools.
- Breach notification procedures: Documented processes for detecting, investigating, and reporting PHI breaches within the 60-day window required by the Breach Notification Rule.
Data minimization: Systems should collect and process only the PHI strictly necessary for their stated function, not everything available.
The most frequent violations include sharing patient data with advertising or analytics platforms without authorization, using non-HIPAA-compliant video conferencing tools for clinical sessions, failing to execute BAAs with sub-processors, storing PHI in unencrypted databases, and lacking audit logs for data access events. Each category carries penalties ranging from $100 to $50,000 per violation per year.
Not all online telemedicine platforms are telehealth platforms HIPAA compliant by design. A platform can offer video sessions and scheduling without meeting the technical and administrative safeguards HIPAA mandates. A HIPAA-compliant telehealth platform has end-to-end encryption, role-based access controls, audit logging, signed BAAs with all sub-processors, and documented incident response procedures built into the architecture.
For a production-grade platform with video sessions, therapist matching, secure messaging, and EHR integration, expect 4–6 months with a specialist healthcare mobile app development company. Platforms attempting to shortcut the compliance architecture phase consistently take longer overall due to rework and face significantly higher risk during that extended timeline.
HIPAA Compliant Applications are healthcare apps designed to securely manage patient data (PHI) while meeting strict privacy and security standards.
They help protect sensitive healthcare data, ensure legal compliance, and build trust with patients and providers.
Essential features include data encryption, secure authentication, role-based access control, audit logs, and secure data storage.
Building HIPAA Compliant Applications involves secure architecture, encrypted data handling, compliance-ready cloud services, and regular security testing.
The Best HIPAA Compliant Mobile Apps for Therapists offer secure messaging, video consultations, appointment scheduling, and encrypted patient records.
Costs vary depending on features and complexity, but are generally higher due to strict security and compliance requirements.
Typically, it takes around 3–9 months based on the app’s scope and integrations.
Yes, startups can build HIPAA Compliant Applications using secure frameworks, cloud platforms, and experienced development teams.
Challenges include ensuring data security, meeting regulatory standards, and maintaining ongoing compliance.
Yes, regular updates, monitoring, and security audits are necessary to stay compliant and secure.
Pallabi Mahanta, Senior Content Writer at Tech Exactly, has over 5 years of experience in crafting marketing content strategies across FinTech, MedTech, and emerging technologies. She bridges complex ideas with clear, impactful storytelling.



