Top 10 Technologies Transforming Healthcare Mobile App Development in 2026

Key Takeaways:
Healthcare apps are evolving into real-time, predictive care systems
AI is delivering near-clinical-grade accuracy and 50% efficiency gains in core workflows
Continuous monitoring via IoT and wearables is reducing hospitalisations and enabling early intervention
Without cloud and EHR interoperability, even well-built apps fail in real clinical environments
In healthcare, poor early architecture decisions create irreversible compliance and scaling risks
The global digital health market is supposed to reach USD 946.04 billion in 2030, and the engine behind that growth isn’t just more apps. It’s the convergence of AI, IoT, cloud infrastructure, and wearable technology that is fundamentally changing how care is delivered, monitored, and personalized at scale.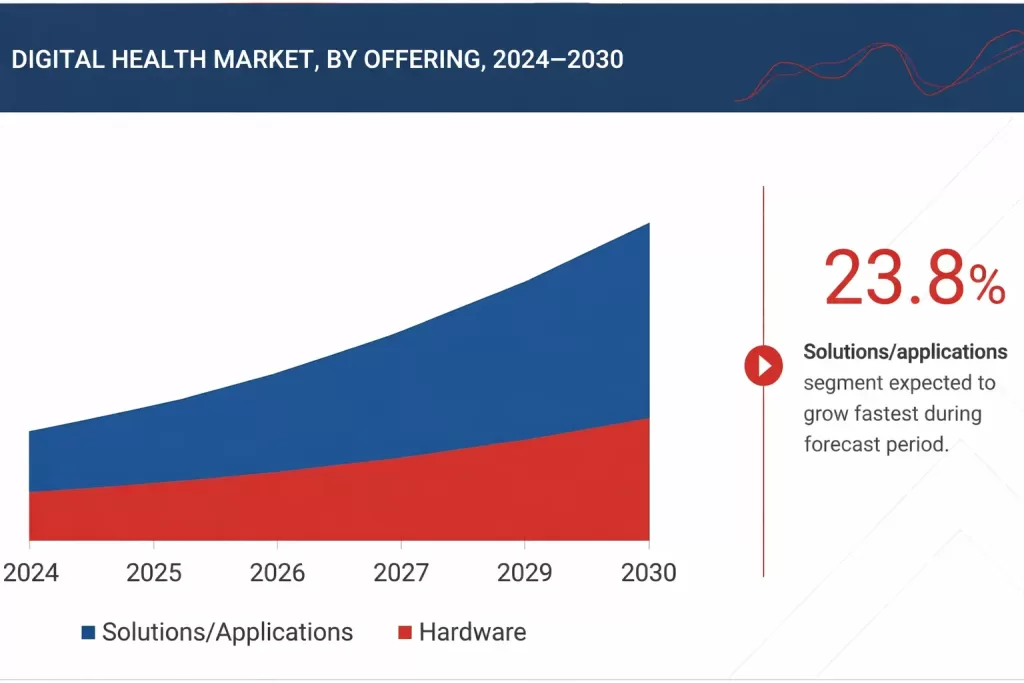
Image source
Healthcare is shifting enterprises from reactive to predictive care models. Now, AI and IoT automation are optimizing clinical workflows and operational efficiency at scale. Interoperable health data platforms are eliminating silos and improving decision-making.
For any healthcare mobile app development company, whether operating as a Healthcare App Development Company in USA or a Healthcare App Development Company in UK, the technology decisions made during the architecture phase directly determine clinical outcomes, compliance posture, and how well the product scales.
This blog breaks down the 10 technologies actively reshaping healthcare mobile app development in 2026, what they do in practice, and what they look like inside real products.
1. Artificial Intelligence: From Diagnostics to Clinical Decision Support
Artificial intelligence is increasingly the core intelligence that makes the product work. AI algorithms now achieve 97.5% accuracy in detecting lung nodules from CT scans, exceeding experienced radiologists at 96.2%, and when combined, accuracy rises to 99.1%. (Source).
In healthcare mobile app development, AI is applied across three primary functions:
Diagnostic support: Image recognition models that analyze radiology scans, dermatology images, and pathology slides, surfacing findings faster than manual review and at a fraction of the cost.
Predictive analytics: Risk stratification models that identify high-risk patients before acute events occur, enabling earlier, cheaper intervention.
Clinical documentation: Ambient AI systems that transcribe and structure clinical conversations in real time, reducing documentation burden on clinicians by 30–50%.
Technology Used: Machine learning frameworks (TensorFlow, PyTorch), NLP models (GPT-4, Claude), computer vision APIs, FHIR-compliant data pipelines.
Real-world example: At Tech Exactly, we built a smart fitness platform that functions as a personal trainer — generating adaptive workout programs and real-time coaching based on individual user performance data
→ Read the Smart Fitness App Case Study
2. Internet of Things (IoT): Continuous Monitoring Beyond the Clinic Walls
The IoT market is projected to cross USD 5,552.48 billion by 2034, with healthcare among the highest-impact sectors for connected device adoption. The applications of IoT in healthcare have moved well beyond hospital asset tracking; IoT now sits at the centre of how technology in healthcare management is being reimagined.
With IoT-enabled devices and wearables, doctors can track patients’ vitals such as heart rate, blood pressure, and glucose levels in real time, enabling early detection of health issues and reducing the need for frequent hospital visits.
Key applications of IoT in healthcare in 2026:
Remote Patient Monitoring (RPM): Continuous vital sign transmission from patient homes to clinical dashboards, enabling intervention before hospitalization becomes necessary. IoT-enabled RPM has been shown to reduce hospital readmissions by up to 47%.
Smart hospital infrastructure: Connected beds with fall detection, RTLS systems tracking equipment and staff in real time, and automated inventory management for high-value medical supplies.
Medication adherence monitoring: Smart dispensers and connected pill bottles that log dosing events and flag missed doses to care teams automatically.
Technology Used: MQTT protocol for device communication, AWS IoT Core or Azure IoT Hub, edge computing nodes for real-time local processing, HL7 FHIR for clinical data exchange.
Related reading → The Future of AI in Healthcare Apps
3. Cloud Computing: The Infrastructure Layer Every Healthcare App Runs On
Modern healthcare tech solutions require infrastructure that scales elastically, maintains near-perfect uptime, and enforces the access controls HIPAA mandates. On-premises hardware cannot reliably deliver any of these at scale. Cloud computing in healthcare ensures a certain level of interoperability: allowing secure, on-demand access to data and enabling healthcare systems to store and share patient information across departments and organizations while remaining compliant with privacy standards.
What cloud infrastructure specifically enables in healthcare mobile app development:
HIPAA-eligible environments: AWS, Azure, and Google Cloud all offer healthcare-specific cloud configurations with Business Associate Agreements, encryption at rest and in transit, and audit logging built into the platform layer.
FHIR-native APIs: Cloud-hosted FHIR R4 services allow healthcare apps to query and exchange patient data across EHR systems without building bespoke integration middleware for every connection.
Scalable AI inference: Running diagnostic AI models in production requires compute that scales with demand; cloud infrastructure provides this without the capital cost of on-premises GPU clusters.
Technology Used: AWS (GovCloud for the highest compliance requirements), Google Cloud Healthcare API, Azure Health Data Services, Terraform for infrastructure-as-code, Kubernetes for container orchestration.
For healthcare mobile app development services targeting both US and UK markets, choosing a cloud provider with data residency options across both jurisdictions is essential to satisfy HIPAA on the US side and UK GDPR on the other, without duplicating your infrastructure investment.
4. Wearable Technology: Clinical-Grade Data from Consumer Devices
Wearable tech in healthcare has moved far beyond step counting. In 2026, clinical-grade wearables are generating physiological data that directly informs treatment decisions, and the healthcare mobile app development layer connecting these devices to clinical workflows is where the product value is created and sustained.
Smart devices now transmit encrypted biometric data in real time, enabling targeted virtual consultations and meeting strict regulatory standards, including HIPAA, without ambiguity.
Current categories of wearable tech in healthcare integrated into mobile platforms:
- Continuous glucose monitors (CGMs): Real-time blood glucose tracking for diabetic patients, with configurable alert thresholds that notify both patient and clinician when intervention thresholds are crossed.
- Cardiac monitoring wearables: FDA-cleared ECG patches and smartwatches capable of detecting atrial fibrillation continuously, rather than only during a scheduled clinical visit.
- Biosensor patches: Adhesive monitors tracking temperature, respiratory rate, and oxygen saturation are widely used in post-surgical recovery and chronic disease management programs.
Technology Used: Bluetooth Low Energy (BLE) and ANT+ for device communication, HealthKit (iOS) and Health Connect (Android) for platform integration, custom SDK development for proprietary device pairing.
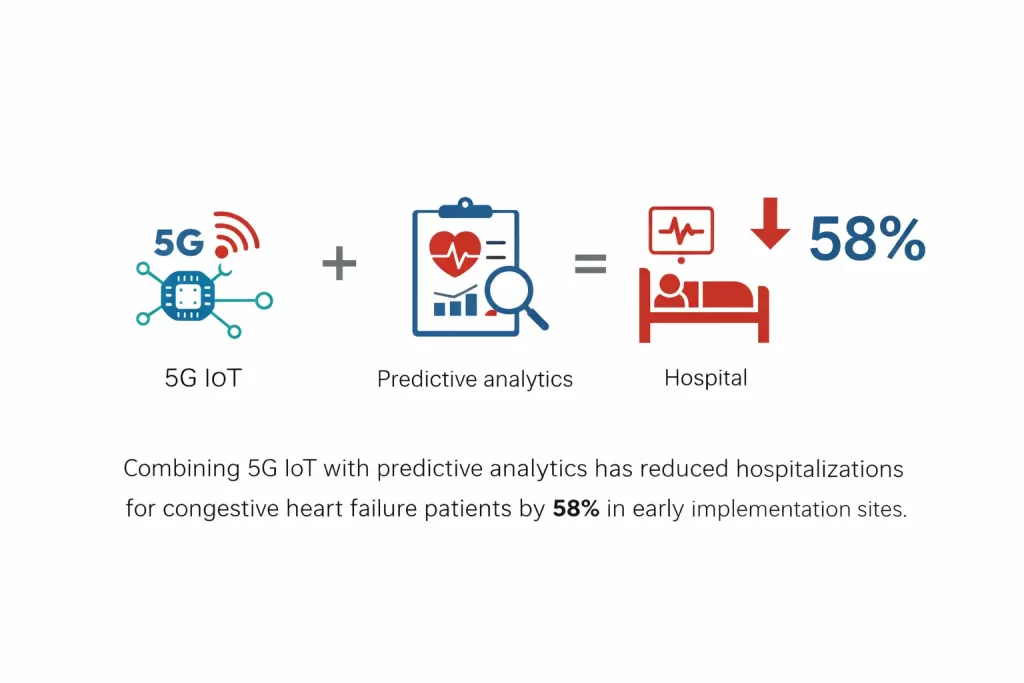
Related reading → How Healthcare Startups Can Build Regulatory-Compliant Apps Without Slowing Innovation
5. Online Telemedicine Platforms That Are Clinically and Legally Sound
Telehealth has stabilized at usage levels 38 times higher than pre-pandemic baselines, and the infrastructure behind reliable online telemedicine platforms is considerably more complex than a video call. It’s a compliance-first architecture that connects clinical workflows, EHR systems, secure messaging, and scheduling into a single, auditable platform.
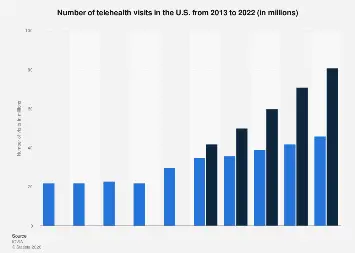
Technology Used: HIPAA-compliant WebRTC providers (Daily.co, Twilio Video), FHIR R4 for EHR data exchange, end-to-end encrypted messaging infrastructure, React Native for cross-platform mobile delivery.
Tech Exactly Case Study: We built a HIPAA-compliant online therapy platform for a New York City mental health practice, connecting patients with therapists via secure audio and video sessions, with integrated scheduling, encrypted asynchronous messaging, and a therapist matching system. Every third-party integration: video provider, cloud host, email notification service required a signed Business Associate Agreement before being connected to patient data.
Every failed login attempt, every data access event, and every session initiation was logged to an immutable audit trail. The result was a platform that delivered clinical-grade security without sacrificing the UX simplicity that mental health patients need.
→ Read the full HIPAA-compliant therapy platform case study
6. EHR Integration for Modern Healthcare Technology
EHR integration is what separates a healthcare app that works in isolation from one that fits into existing clinical workflows. Without it, even well-designed products become parallel systems that clinicians maintain alongside their existing tools and eventually abandon.
EHR systems examples commonly integrated into healthcare mobile app development projects include Epic, Cerner (Oracle Health), athenahealth, and SimplePractice for behavioral health. The integration standard in 2026 is FHIR R4 mandated for certified EHR systems under the ONC’s 21st Century Cures Act final rule.
- Scoped FHIR queries request only the specific data resource a task requires, creating an auditable data minimization record relevant to both HIPAA and UK GDPR compliance.
- SMART on FHIR enables single sign-on authentication for clinical app launches directly from within the EHR interface, significantly improving clinician adoption.
- Bidirectional FHIR integration allows apps to write structured data back to the EHR, closing the loop between app-generated insights and the clinical record.
Technology Used: HL7 FHIR R4, SMART on FHIR for authentication, Mirth Connect or Microsoft Azure FHIR service for integration middleware, Epic App Orchard or Cerner Code for certified EHR app deployment.
This is an area where technology in healthcare management is evolving fastest, moving from point-to-point integrations to ecosystem-level interoperability that enables care coordination across organizational boundaries.
7. Blockchain: Immutable Data Provenance for Health Records and Consent Management
In large health networks and medical tech lab environments, blockchain addresses one of the most persistent problems in technology in the healthcare sector: sharing patient data across organizations while maintaining an immutable audit trail and verifiable patient consent record.
Blockchain in healthcare is applied to three primary use cases:
Consent management: Patient authorization for data sharing is recorded on an immutable ledger, providing a tamper-proof record of exactly what was consented to and when, relevant to both HIPAA authorization requirements and GDPR consent obligations.
Drug supply chain integrity: Pharmaceutical provenance tracked from manufacturer to dispensing point, reducing counterfeit drug exposure and improving recall efficiency.
Cross-institutional data sharing: Federated patient record access across health systems without a central data repository, reducing breach surface area while improving care coordination.
Technology Used: Hyperledger Fabric for permissioned enterprise healthcare networks, Ethereum for public-chain consent applications, IPFS for distributed health record storage.
📝Note: Blockchain isn’t appropriate for every healthcare application, but for healthcare tech solutions requiring auditable data provenance across organizational boundaries, it provides technical guarantees that no centralized database can replicate.
8. Augmented Reality and Virtual Reality: Precision Surgery and Therapeutic Applications
The healthcare AR/VR market is poised to become a USD 38.0 billion market with applications spanning surgical precision, medical education, and patient therapy.
In healthcare mobile app development, AR and VR serve distinct but complementary functions across the care continuum:
- Surgical planning and guidance: AR overlays patient imaging data onto the surgical field in real time, giving surgeons anatomical reference during procedures and reducing intraoperative errors.
- Clinical training and simulation: VR environments where medical students and clinicians practice complex procedures without patient risk, compressing the learning curve for high-stakes interventions.
- Therapeutic applications: VR-based pain management for burn patients, exposure therapy for PTSD and phobias, and cognitive rehabilitation for neurological conditions, all with documented clinical efficacy.
Technology Used: Unity3D and Unreal Engine for VR environment development, ARKit (iOS) and ARCore (Android) for mobile AR, Microsoft HoloLens for surgical AR overlay, and OpenXR for cross-platform VR deployment.
Related reading → Agentic AI in Healthcare: How Autonomous Systems Are Transforming Patient Care
9. Generative AI for Clinical Documentation and Patient Engagement
Healthcare’s transition from volume to value requires access to longitudinal data, care coordination across teams, and real-time monitoring, and generative AI is increasingly the technology enabling each of these at a clinical scale.
In healthcare mobile app development specifically, generative AI is being deployed across three high-value functions:
- Ambient clinical documentation: AI systems that listen to patient-clinician conversations and generate structured clinical notes in real time. Reducing documentation time by 30–50% and returning clinician attention to the patient.
- Personalized patient education: Plain-language explanations of diagnoses, medications, and care plans generated from structured clinical data, adapted to individual health literacy levels automatically.
- Intelligent pre-consultation triage: Conversational AI systems that conduct symptom assessment, structure patient history, and flag high-acuity cases before the clinician joins the session.
Technology Used: OpenAI GPT-4o or Anthropic Claude via API, fine-tuned clinical LLMs for domain-specific accuracy, FHIR-integrated output pipelines for structured note generation, RAG (Retrieval-Augmented Generation) for grounding outputs in patient-specific context.
For any Healthcare App Development Company in USA or Healthcare App Development Company in UK deploying generative AI in a clinical context, output governance: bias monitoring, human review gates, and audit logging of AI-generated content is as important as the model itself.
Related reading → Healthcare App Development in 2026: What Actually Goes Into Building a Compliant Product
10. 5G Connectivity: The Network Layer That Makes Real-Time Healthcare Possible
5G isn’t just faster internet; it’s the backbone of the future of healthcare mobile apps. Real-time consultation without lag, massive MRI scan transfer as easily as a text message. This level of instant, high-volume data exchange is becoming the standard for patient care in 2026.
The impact on healthcare mobile app development is most significant in three areas:
- Real-time remote care: Sub-10ms latency enabling remote specialist consultation with high-resolution imaging, robotic-assisted procedures, and ambient monitoring applications that were technically impossible on 4G.
- Dense IoT environments: 5G supports up to 1 million connected devices per square kilometer, enabling the fully instrumented hospital environments that applications of IoT in healthcare require at an enterprise scale.
- Edge AI processing: 5G enables AI inference to run at the network edge rather than the cloud, reducing latency for real-time diagnostic applications and keeping more patient data local to the care setting.
Technology Used: 5G-enabled device SDKs, Mobile Edge Computing (MEC) platforms, WebRTC with 5G optimization for telehealth video, Azure Edge Zones, or AWS Wavelength for healthcare edge deployments.
Choosing a Healthcare Mobile App Development Partner Who
Understands the Full Stack
The 10 technologies above don’t work in isolation. The healthcare products that deliver genuine clinical value are the ones where AI, IoT, cloud infrastructure, EHR integration, and compliance architecture are designed together from the first sprint.
A healthcare mobile app development company that understands how these technologies intersect and how compliance requirements shape every integration decision will produce fundamentally different outcomes than a generalist team treating healthcare as a standard mobile build.
Whether you’re engaging a Healthcare App Development Company in USA for a HIPAA-regulated telehealth platform, a Healthcare App Development Company in UK building to NHS Digital standards, or a global medical tech lab exploring both markets, the technology decisions made in the first two weeks of architecture have more impact on long-term product quality than anything that follows.
At Tech Exactly, our healthcare mobile app development services are structured around this principle. Every healthcare engagement begins with a compliance and technology architecture review before any feature scoping. If you’re building in the healthcare space and want to understand which of these technologies belong in your product and how to integrate them without creating regulatory or technical debt, we can connect and help you plan it.
Let's Start Your Project Today
Ready to build your App with us? Reach out now – our experts are just one click away.
Frequently Asked Questions
The foundational technology stack for healthcare mobile app development in 2026 includes:
- AI/ML for diagnostics and documentation
- IoT for remote patient monitoring
- Cloud infrastructure for HIPAA-compliant data management
- EHR integration via FHIR R4, wearable tech connectivity
- Generative AI for clinical workflow automation
The right combination depends on your specific use case: a telehealth platform has different technology priorities than a wearable monitoring application or a clinical decision support tool.
The primary applications of IoT in healthcare are remote patient monitoring (continuous vital sign transmission from patient homes to clinical dashboards), smart hospital infrastructure (connected beds, equipment tracking, automated inventory), and medication adherence monitoring (smart dispensers that log dosing events and flag missed doses). All three require careful data pipeline architecture, edge computing capability, and HIPAA-compliant transmission protocols to function reliably in a clinical setting.
Wearable tech in healthcare generates continuous physiological data from CGMs, cardiac monitors, and biosensor patches that is surfaced to patients and clinicians through mobile app interfaces. The mobile layer handles data visualization, alert management, and clinical communication, while the backend pipeline manages device pairing, BLE data ingestion, and EHR synchronization.
- Look for demonstrated experience with HIPAA-compliant architecture, FHIR R4 integration, and a development process that treats compliance as an architectural requirement rather than a post-launch review.
- Ask for specific examples of EHR integrations they've delivered, how they handle BAA coverage across third-party vendors, and what their audit logging architecture looks like for a production healthcare application.
A team that can answer those questions specifically, not generically, has built in this space before.
Pallabi Mahanta, Senior Content Writer at Tech Exactly, has over 5 years of experience in crafting marketing content strategies across FinTech, MedTech, and emerging technologies. She bridges complex ideas with clear, impactful storytelling.

