Telemedicine App Development in 2026: Features, Compliance, Cost, and the Timeline Nobody Warns You About

Key Takeaways
- The telemedicine market is projected to hit $380 billion by 2030 — but capturing that opportunity requires building the compliance and EHR architecture before writing a single feature.
- Using Zoom or any generic video tool without a Business Associate Agreement in place is a HIPAA violation, regardless of how encrypted it is.
- A full telemedicine platform with EHR integration realistically takes 6–9 months from scoping to production launch — not the 90-day MVP timeline most founders budget for.
- Teams that invest in cross-platform development (React Native or Flutter) ship 30–40% faster than those building separate native codebases, without meaningful performance trade-offs for most telemedicine use cases.
7 million prescriptions for controlled substances were issued through telemedicine in 2024, all without a single in-person visit. The DEA (Drug Enforcement Administration) has further extended the temporary telemedicine flexibilities, including prescribing controlled substances, through 2026. That means the window for building a telemedicine app is wide open.
There are many things that most telemedicine app development guides do not cover. Features such as video calls, e-prescribing, and secure messaging are the easy part. The challenge is to build an app that complies with HIPAA and navigates the DEA’s shifting prescribing rules. Additionally, the app should integrate with the EHR systems your clients actually use. And yet, it should feel simple enough that a 72-year-old patient in rural Arkansas can figure it out on her first try.
The global telehealth market is projected to reach $459.8 billion by 2030, with 94% of telehealth patients saying that they would use it again. However, the market isn’t really rewarding to every telehealth app. It rewards those apps that solve real clinical workflow problems. Not the ones that just add a video call feature to the booking system and portray it as an innovation.
As a healthcare app development company, we have been building healthcare apps, including telemedicine platforms, patient portals, remote monitoring systems, and EHR integrations, for over a decade. This guide has everything you need to build a telemedicine application. From features that drive clinical adoption, compliance architecture for legality, to what it actually costs, and the development timeline you should actually consider.
Telemedicine vs. Telehealth: How They Differ
Before we dive into features and costs, it’s important to clear confusion that directly affects the scope decisions. Telemedicine and telehealth aren’t the same things. However, most people, including development teams, use them interchangeably.
Telemedicine refers specifically to remote clinical services: video consultations, remote diagnosis, e-prescribing, and clinical decision-making between a provider and patient.
Telehealth is broader. It includes telemedicine plus non-clinical services like provider training, administrative meetings, continuing medical education, and public health monitoring.
And why does it matter to you? When building a telemedicine app, your compliance scope is more specific (HIPAA, DEA, state medical board licensing). Your feature set is more clinically focused, and your EHR integration requirements are rigorous. So, it’s important to know what you are building before scoping out the requirements.
Core Features of a Telemedicine App That Clinicians Actually Adopt
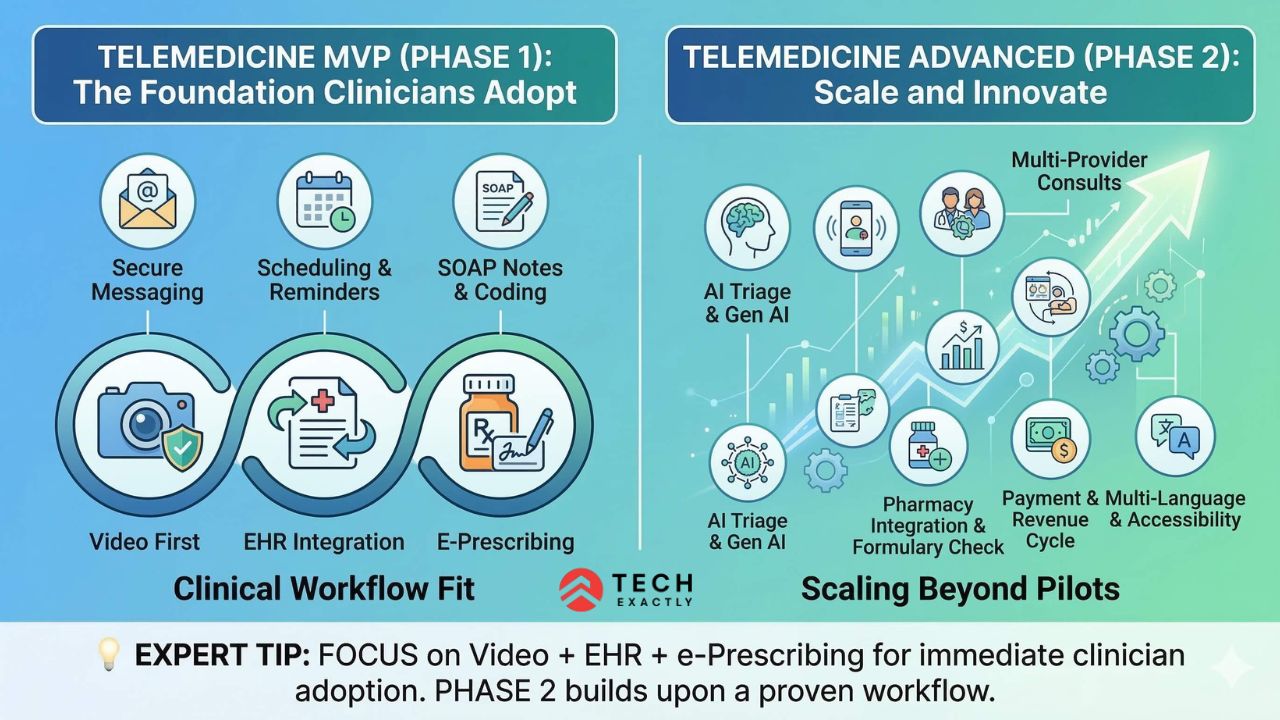
The difference between a telemedicine app that becomes part of everyday clinical workflows and one that gets abandoned after the pilot phase usually comes down to one thing: features that solve real problems. Not flashy features designed only to impress providers during a demo.
Must-Have Features (MVP)
Feature | What It Does | Why It Matters |
HIPAA-Compliant Video Visits | End-to-end encrypted live video between patient and provider with screen sharing and virtual waiting room | It is the core of the product. Must support even low-bandwidth connections, as millions of Americans lack access to reliable broadband. |
Secure Messaging | Async text and media communication between the care team and patient | Not every clinical question needs a video call. Messaging handles 40-60% of follow-up interactions |
E-Prescribing (EPCS) | Electronic prescribing, including controlled substances, with DEA-compliant digital signatures | DEA flexibilities allow Schedule II-V prescribing via telehealth through Dec 2026. Build this capability now while the window is open |
Appointment Scheduling | Self-service booking with provider availability, automated reminders, and waitlist management | Telehealth is associated with a 29% reduction in no-show odds. Patients expect Calendly-level simplicity from their healthcare provider |
EHR Integration | Bi-directional data exchange with Epic, Oracle Health, athenahealth, or other EHR systems | Without this, providers have to document visits in two systems. That kills adoption faster than any UX issue |
Clinical Documentation | Visit notes, SOAP templates, diagnosis coding (ICD-10), and procedure coding (CPT) | Providers won’t use an app that adds documentation burden. Auto-populated fields from intake forms save 5-10 minutes per visit |
Patient Intake & Consent | Digital forms for demographics, insurance, medical history, and telehealth consent | Eliminates pre-visit phone calls. Consent documentation is legally required for telehealth in most states |
Advanced Features (Phase 2+)
Feature | What It Does | Why It Matters |
AI-Powered Symptom Triage | Pre-visit assessment that routes patients to the appropriate care level | Reduces unnecessary ER visits. Generative AI is transforming clinical triage workflows |
Remote Patient Monitoring Integration | Connect wearables and medical devices for continuous vitals tracking | Critical for chronic disease management, which helps turn episodic telehealth into continuous care. RPM apps integrate naturally with telemedicine platforms |
Multi-Provider Consultations | Group video for specialist referrals, care team huddles, and family conferences | Essential for behavioral health, oncology, and complex care coordination |
Pharmacy Integration | Real-time formulary checks, medication interaction alerts, prescription routing | Reduces prescribing errors and patient callbacks about medication issues. See our pharmacy app development guide |
Payment Processing | Co-pay collection, insurance verification, and superbill generation | Revenue cycle matters. Collecting payment at the time of service improves collection rates by 30%+ |
Language & Accessibility | Multi-language support, real-time translation, ADA-compliant UI, closed captions on video | Health literacy gaps disproportionately affect the populations telehealth is meant to serve |
💡 Expert Tip: Build your MVP around this trio – video first + EHR integration + e-prescribing. That’s the MVP that the providers will adopt and switch their workflows for. Everything else, like AI triage, RPM, and multi-provider, can wait and instead be a part of Phase 2 after you have proven clinical workflow fit. Apps that try to launch with every other feature fail because not everything works well, and in the end becomes chaos.
The Compliance Architecture for Telemedicine App Development
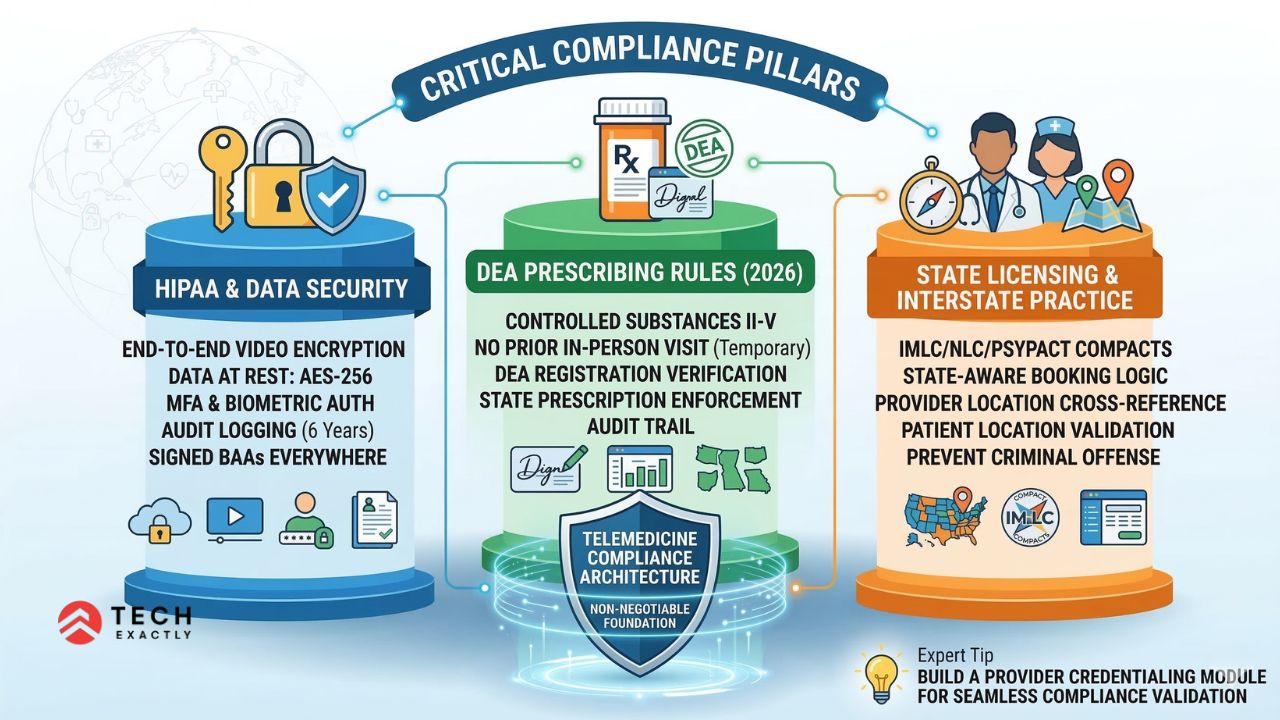
Telemedicine operates at the intersection of healthcare regulations, controlled substance laws, and state-level licensing rules. Get any one of these wrong, and your app is either illegal, uncertifiable, or both.
HIPAA: The Non-Negotiable Foundation
Every telemedicine app handles Protected Health Information (PHI), which means HIPAA compliance is mandatory, not optional.
Video encryption: End-to-end encryption for all video, audio, and screen sharing. Consumer platforms like FaceTime and standard Zoom do not meet HIPAA requirements. Thus, you need a HIPAA-eligible video infrastructure with a signed BAA.
Data at rest: AES-256 encryption for all stored PHI —that translates to visit recordings (if enabled), clinical notes, messages, and audit logs.
Authentication: MFA for all users. Biometric login for mobile. OAuth 2.0 / SAML for SSO with hospital identity providers.
Audit logging: All PHI access must be logged, including who accessed what, when, and from where. Logs must be tamper-proof and retained for a minimum of 6 years.
BAAs everywhere: Any third-party service that touches PHI requires a signed Business Associate Agreement. This applies to all features and core functionality, including cloud hosting, video infrastructure, push notifications, analytics, and payment processing.
▶️ Learn how Tech Exactly built a HIPAA-compliant platform for an NYC therapy practice
DEA Telehealth Prescribing Rules (2026)
If your telemedicine app includes e-prescribing for controlled substances, you are operating under the DEA’s telehealth flexibilities, and these rules are in transition.
What’s currently allowed (through December 31, 2026):
DEA-registered practitioners can prescribe Schedule II-V controlled substances via audio-video telemedicine without requiring a prior in-person visit under the fourth temporary extension
Schedule III-V medications for opioid use disorder (buprenorphine) can be prescribed via audio-only encounters
What your app needs to support:
DEA-compliant Electronic Prescribing for Controlled Substances (EPCS) with two-factor authentication and digital signatures
Provider DEA registration verification
State-level prescribing rules enforcement (some states, like New York and New Jersey, have stricter rules than federal flexibilities)
Audit trail for every controlled substance prescription
⚠️ Reality Check: If you are building a telemedicine app that includes controlled substance prescribing, build your app to adapt to both present and future regulations and the Ryan Haight Act’s original in-person visit requirement. This will help you future-proof your app regardless of which direction the permanent rules go.
State Licensing and Interstate Practice
A telehealth appointment happens in the state where the patient is located and not where the provider is licensed. This results in a multi-state challenge that your app must address.
Interstate licensing compacts that simplify this:
IMLC (Interstate Medical Licensure Compact): Expedited pathway for physician licensure across participating states
NLC (Nurse Licensure Compact): Multi-state nursing practice under a single license
PSYPACT: 43 states now participate in the psychology interjurisdictional compact — the most mature telehealth compact
Your app needs state-aware logic that validates whether a provider is licensed to treat a patient in their specific state, and blocks appointments where licensing doesn’t exist. This is not just a nice-to-have feature. In case you are practicing without a license in the patient’s state, it will result in a criminal offense in most jurisdictions.
💡 Expert Tip: Build a provider credentialing module that stores each provider’s state licenses, DEA registrations, and compact memberships, then cross-references them against the patient’s location at the time of booking. This helps prevent compliance violations while reducing the manual credentialing work operations teams deal with every day.
Let's Start Your Project Today
Ready to build your Telemedicine app with us? Reach out now – our experts are just one click away.
Telemedicine App Development Cost Breakdown
There’s a common question that every founder and CTO asks: how much does telemedicine app development cost? The answer largely depends on two major cost drivers: video infrastructure and EHR integrations.
Let’s take the business case first. A Telehealth visit is cheaper and takes less time for the patients. Plus, a systematic review of 77 studies during COVID-19 found clinical outcomes between telehealth and in-person care were “generally not clinically meaningful” in difference. Translation: same outcomes, half the cost, a fraction of the friction. That’s the ROI context for the numbers below.
Cost by Complexity Tier
Portal Complexity | What’s Included | Estimated Cost | Timeline |
Basic Telemedicine App | 1:1 video visits, secure messaging, appointment scheduling, and patient intake. Single-platform (web or mobile). HIPAA-compliant hosting. No EHR integration. | $65,000 – $120,000 | 3-5 months |
Mid-Range Platform | Everything above + EHR integration (1-2 systems), e-prescribing (non-controlled), clinical documentation, insurance verification, iOS + Android apps. | $150,000 – $280,000 | 5-8 months |
Enterprise Platform | Full feature set + EPCS for controlled substances, multi-provider video, RPM integration, AI triage, white-label/multi-tenant, advanced analytics, and wearable integration. | $300,000 – $500,000+ | 8-14 months |
Where the Money Actually Goes
Cost Component | % of Total Budget | Why |
Video Infrastructure | 20-30% | Real-time video is technically demanding — WebRTC implementation, TURN/STUN servers, adaptive bitrate, recording, and low-bandwidth fallback. This is the core product and the hardest to get right. |
EHR Integration | 20-30% | Each EHR system (Epic, Oracle Health, athenahealth) has its own FHIR/HL7 implementation quirks. Multiple integrations multiply the cost linearly. |
Compliance & Security | 15-20% | HIPAA architecture, penetration testing, EPCS certification, audit logging, encryption infrastructure, DEA compliance, and state licensing logic. |
Frontend Development | 10-15% | Patient app, provider app, admin dashboard. Responsive web + mobile (iOS/Android). |
Backend / API Layer | 10-15% | Business logic, scheduling engine, notification services, payment processing, prescription routing. |
UX/UI Design | 5-8% | Clinical workflow mapping, patient experience research, accessibility (WCAG 2.1 AA), prototype testing. |
QA & Testing | 5-8% | Video quality testing across devices/networks, compliance validation, interoperability testing, and load testing for concurrent video sessions. |
Cost Variables That Shift the Number
Video infrastructure choice: Building on WebRTC from scratch vs using Daily.co, Vonage or LiveKit can help SDKs save 2-3 months of development but add per-minute usage costs ($0.004-$0.01/participant/minute).
Number of EHR integrations: Each additional EHR adds $25,000-$60,000. Epic alone requires a separate App Orchard review process.
Mobile app approach: Native iOS + Android adds $50,000-$100,000 over web-only. Cross-platform frameworks like React Native or Flutter cut that by 30-40%.
EPCS certification: Adding DEA-compliant electronic prescribing for controlled substances requires identity proofing integration (e.g., Exostar, IdenTrust) and adds $15,000-$30,000.
AI features: AI-powered functionality like symptom triage, clinical note summarization, or agentic AI workflows in healthcare apps add $30,000-$70,000, depending on complexity.
Multi-tenant architecture: Building for multiple provider organizations (SaaS model) adds 15-20% to total cost.
Ongoing costs: HIPAA-eligible cloud hosting ($2,000-$8,000/month), video infrastructure usage fees, EPCS subscription, third-party API costs, maintenance, and support.
For a broader perspective on healthcare app costs across all categories, see our healthcare app development cost guide.
Let's Start Your Project Today
Ready to build your Telemedicine app with us? Reach out now – our experts are just one click away.
Telemedicine App Development Timeline: Phase by Phase
Here’s what a realistic timeline looks like for a mid-range telemedicine platform with EHR integration and mobile apps:
Phase | Duration | Key Activities |
Phase 1: Discovery & Compliance Scoping | 3-4 weeks | Requirements gathering, regulatory assessment (HIPAA, DEA, state licensing), EHR integration scoping, video infrastructure evaluation, security architecture planning |
Phase 2: UX Design & Clinical Workflow Mapping | 4-6 weeks | User research with providers AND patients, video visit flow design, clinical documentation templates, wireframing, prototype testing, WCAG accessibility audit |
Phase 3: Backend & Video Infrastructure | 8-12 weeks | Core API development, video infrastructure (WebRTC/SDK integration), scheduling engine, authentication/authorization, encryption infrastructure, notification services |
Phase 4: Frontend Development | 6-10 weeks | Patient-facing web + mobile apps, provider-facing app, admin dashboard, real-time video UI, offline-capable architecture for low-connectivity scenarios |
Phase 5: EHR Integration & E-Prescribing | 4-8 weeks | EHR sandbox testing, FHIR/HL7 middleware, e-prescribing integration, pharmacy network connectivity, clinical data synchronization |
Phase 6: Security & Compliance Testing | 3-5 weeks | Penetration testing, HIPAA compliance validation, EPCS certification testing, video quality assurance across devices/networks, load testing |
Phase 7: Launch & Post-Launch | 2-3 weeks | Staged rollout, monitoring setup, incident response activation, provider training, patient onboarding materials |
Total: 5-8 months for a mid-range platform. Enterprise builds with multiple EHR integrations and EPCS: 8-14 months.
⚠️ Reality Check: The two biggest timeline killers in telemedicine app development are EHR credentialing (getting production API access from Epic or Oracle Health can take 4-8 weeks after application) and EPCS certification (identity proofing vendor integration adds 2-4 weeks). Focus on building these into your project plan from day one rather than adding them later
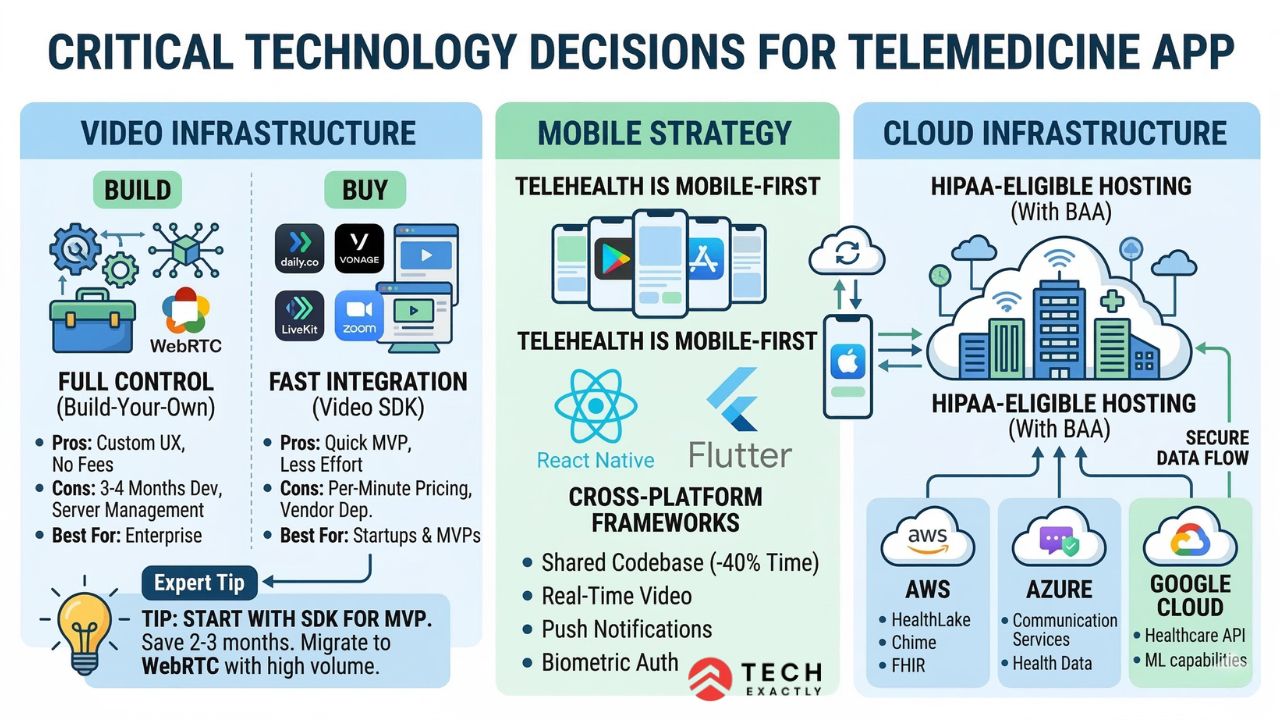
Technology Decisions That Shape Your Telemedicine App
Video Infrastructure: Build vs. Buy
This is the single biggest technology decision in telemedicine app development.
Approach | Pros | Cons | Best For |
WebRTC (Build) | Full control, no per-minute fees, custom UX | 3-4 months of development, TURN/STUN server management, cross-browser testing | Enterprise platforms with high volume and custom requirements |
Fast integration, pre-built UI components, HIPAA-eligible with BAA | Per-minute pricing, vendor dependency | MVPs and startups prioritizing speed | |
Vonage / LiveKit | Programmable video APIs, HIPAA-eligible, strong documentation | Less pre-built UI, per-minute pricing | Mid-range platforms needing customizable video |
Zoom Video SDK | Brand recognition, reliable infrastructure | Higher cost, limited customization for clinical workflows | Organizations already using Zoom for Healthcare |
💡 Expert Tip: For most startups, start with a video SDK for your MVP. The per-minute cost of SDKs is negligible at low volume, and you save 2-3 months of WebRTC implementation. Once you’ve validated product-market fit and volume justifies it, migrate to custom WebRTC. Trying to build WebRTC from scratch in v1 is the #1 cause of telemedicine app development delays.
Mobile Strategy
Almost all Americans own a mobile, and patients take video calls from wherever they are. Telehealth is essentially mobile first, and that’s why you need a mobile app.
We recommend React Native or Flutter for telemedicine mobile app development. The shared codebase cuts development time by 30-40%, and both frameworks handle real-time video, push notifications, and biometric authentication well. For a deeper comparison, see our tech stack guide for healthcare apps.
Cloud Infrastructure
Telemedicine hosting must be HIPAA-eligible with a signed BAA. Video adds specific infrastructure requirements:
AWS — Most common. HIPAA-eligible services, Amazon Chime SDK for video, HealthLake for FHIR. Best overall ecosystem for telemedicine.
Azure — Strong Azure Communication Services for video, Azure Health Data Services for FHIR. Good fit for Microsoft-heavy healthcare organizations.
Google Cloud — Healthcare API with FHIR store, strong ML capabilities for AI triage features. WebRTC originated at Google — solid video infrastructure.
What Comes Next
Telemedicine app development is at a crucial turning point. The DEA’s controlled substance prescribing flexibilities have been extended through 2026, but they are still temporary. This further creates an opportunity for platforms that can handle both current and future rules.
At the same time, the physician shortage is projected to reach 86,000 by 2036. Telehealth currently accounts for just 5-6 % of all outpatient visits, and this is projected to rise to 25-30% by 2027. This specifically suggests that telemedicine is not just a convenience play anymore; it is a capacity play. The platforms that win will be the ones that make virtual care as clinically effective as walking into a clinic, with none of the friction.
The tech decisions that you take today, like choosing features such as video infrastructure, EHR integration architecture, compliance, etc., will determine whether your platform scales or stalls. That requires an app development partner who understands clinical workflows, not just video APIs.
If you’re planning a telemedicine app and want to understand what the compliance architecture, integration scope, and realistic cost look like for your specific use case, we offer a free consultation to map it out.
Let's Start Your Project Today
Ready to build your Telemedicine app with us? Reach out now – our experts are just one click away.
Frequently Asked Questions
A basic telemedicine app with video visits, messaging, and scheduling starts at $65,000-$120,000. Mid-range platforms with EHR integration, e-prescribing, and mobile apps run $150,000-$280,000. Enterprise platforms with EPCS, AI triage, RPM integration, and multi-tenant architecture range from $300,000-$500,000+. Cost is driven by two major things: video infrastructure choice (SDK vs. custom WebRTC) and how many EHRs you need to connect. For costs across all healthcare app types, see our cost breakdown guide.
A basic MVP with video visits takes 3-5 months. A mid-range platform with EHR integration and mobile apps takes 5-8 months. Enterprise implementations with EPCS and multiple integrations take 8-14 months. The biggest risk is getting official permissions from vendors. It takes 4-8 weeks to get production API access from Epic or Oracle Health.
HIPAA (Privacy, Security, and Breach Notification Rules) is the bare minimum for apps handling PHI. If your app includes features like controlled substance prescribing, DEA compliance, and EPCS certification becomes mandatory. The state-level telehealth laws vary significantly, and they focus on consent, licensing and prescribing rules. CMS reimbursement rules impact which services are billable through telehealth.
Yes, till December 31, 2026, as per the DEA's fourth temporary extension. Practitioners registered through the DEA can prescribe Schedule II-V controlled substances through audio-video telehealth without requiring a prior in-person visit. But your app must support EPCS with two-factor authentication and meet both federal and state prescribing requirements. Though permanent rules are still being developed.
If you want a faster development, you can go with white-label platforms (Doxy.me, VSee, Mend), although the customization will be limited. If you need deep EHR integration, EPCS for controlled substances, a branded patient experience, specific clinical workflows (dermatology imaging, behavioral health group sessions), or a SaaS product serving multiple provider organizations, a customised telemedicine app development is the best choice. The ROI breakeven for custom development is typically within 18-24 months for organizations doing 500+ telehealth visits per month.
Telemedicine apps focus on remote clinical services like video consultations, diagnosis, and treatment. On the other hand, Telehealth caters to a broader picture and includes non-clinical services like provider training and administrative tools. Telemedicine apps have stricter compliance requirements (HIPAA, DEA, state medical board rules) and more demanding EHR integration needs.
Manas Das, Mobile App Architect at Tech Exactly, has over 9 years of experience leading teams in iOS, Android, and cross-platform development. He specialises in scalable app architecture and GenAI-driven mobile innovation.
